Dear AuntMinnie Member,
It's been an eventful week or so in the world of breast cancer screening. On May 5, the American College of Radiology (ACR) and Society of Breast Imaging (SBI) released updated screening recommendations for women at higher-than-average risk of breast cancer. And then on May 10, the U.S. Preventive Services Task Force (USPSTF) announced new draft recommendations that added its first-ever support for breast cancer screening beginning at age 40 for all women.
Check out our report on the USPSTF recommendations and our video interview with Dr. Carol Mangione, immediate past chair of the USPSTF, for all of the details.
The task force's decision to only recommend biennial screening as of age 40 was disappointing to many screening advocates, however. In another video interview, Dr. Stamatia Destounis from the ACR and Dr. Sarah Friedewald from the SBI discussed their organizations' recently released guidelines and shared their thoughts on the USPSTF's draft recommendations.
Our continuing coverage from the recent SBI annual meeting also generated significant page views this week. Stop by our Women's Imaging Community for our reporting on SBI presentations detailing the risks of lobular carcinoma in situ and highlighting the importance of supplemental screening for finding interval cancers.
3D printing
Although most radiology chief residents haven't received exposure to 3D printing as part of their current curricular and clinical practices, most would prefer to learn about the technology and have it incorporated into their residency experience, according to an article we're featuring in our Advanced Visualization Community.
The researchers hope that their findings will help persuade residency programs and program directors to consider integrating 3D printing training.
Incidental CT lung cancer screening findings
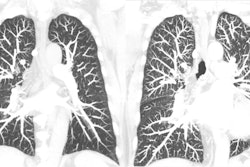
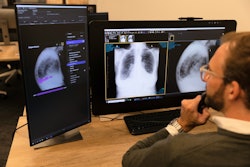
The week of May 8-14 was the American Lung Association's Lung Cancer Action Week, so it was fitting that our top article in the CT Community revealed how radiologists should act when considering how to report significant incidental findings encountered on low-dose CT lung cancer screening exams.
In an analysis of participants in the National Lung Screening Trial, one-third had significant incidental findings on their LDCT study. And nearly 90% of those were considered to be reportable to referring clinicians.
While the researchers acknowledged that the large number of these clinically significant findings may be associated with a heavy burden of follow-up care and testing, they also highlighted the opportunity for early detection of non-lung cancer conditions in high-risk populations and the need for these results to be reported in a consistent manner.