A retrospective analysis of over one million mammograms and over 500,000 digital breast tomosynthesis (DBT) exams published May 30 in Radiology found that DBT yielded more success than digital mammography across multiple screening rounds.
A team led by Brian Sprague, PhD, from the University of Vermont in Burlington found that DBT leads to lower recall rates and could help detect more cancers than mammography across three screening rounds. However, the two modalities did not have any significant differences in interval or advanced cancer detection rates.
"These findings provide new evidence for women, healthcare providers, and policymakers evaluating the benefits, harms, and limitations of multiple rounds of breast cancer screening with DBT compared with digital mammography," Sprague and colleagues wrote.
DBT has been commercially available in the U.S. for more than a decade. An October report found that nearly half of mammography facilities accredited by the U.S. Food and Drug Administration (FDA) use the technology. Previous research suggests that DBT leads to higher cancer detection rates and lower recall rates compared with conventional mammography.
However, the researchers pointed out that cancer detection over multiple rounds is needed to better evaluate DBT's performance. They also noted that "little evidence to date" exists on DBT potentially reducing the incidence of screening failures, including interval or advanced breast cancer.
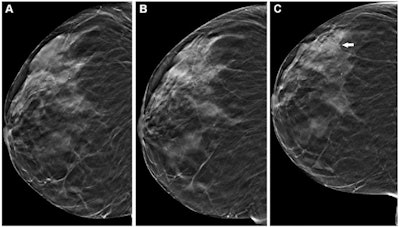 Example images from three successive rounds of DBT show a right craniocaudal tomosynthesis section in a 66-year-old woman screened in (A) 2020, (B) 2021, and (C) 2022 with a new area of architectural distortion identified in 2022 (arrow). This led to a cancer diagnosis. Images courtesy of RSNA.
Example images from three successive rounds of DBT show a right craniocaudal tomosynthesis section in a 66-year-old woman screened in (A) 2020, (B) 2021, and (C) 2022 with a new area of architectural distortion identified in 2022 (arrow). This led to a cancer diagnosis. Images courtesy of RSNA.Sprague and co-authors wanted to compare breast cancer screening outcomes with DBT and mammography on three successive screening rounds.
They collected retrospective data from 58 breast imaging facilities in the Breast Cancer Surveillance Consortium and analyzed outcomes for women ages 40 to 79. The data was recorded between 2011 and 2020. For the study, the team evaluated 523,485 DBT exams and 1,008,123 mammography exams among 504,863 women.
The researchers found that while recall rates decreased with each successive screening round for both modalities, DBT showed significantly lower absolute recall rates per round.
| Recall rates for DBT, mammography in successive screening | |||
| Recall rate (%) | Mammography | DBT | p-value |
| Round one | 10.9 | 7.5 | < 0.001 |
| Round two | 8.6 | 6.9 | 0.003 |
| Round three | 7.3 | 6.1 | 0.03 |
The team also found that DBT had significantly higher cancer detection compared with mammography only for round three and above. This included a difference of 0.6 cancers per 1,000 exams in favor of DBT (p = 0.009).
The researchers also reported no significant differences in interval cancer rate or total advanced cancer rate. They suggested that based on these findings, the possibility of increases in early-stage cancer detection tied to DBT adding to overdiagnosis cannot be ruled out.
However, the study results confirm that DBT has benefits over digital mammography, according to the authors.
"Overall, our results provide support for further dissemination of DBT, tempered by continued uncertainty regarding the effect of DBT on screening failure rates, overdiagnosis, and breast cancer mortality," they wrote.
The team called for more research with larger sample sizes and longer follow-up duration to investigate potential differences in screening failure rates between the two modalities.