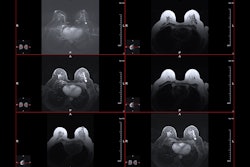
PITTSBURGH – Imaging has an important role in post-surveillance care for breast cancer patients, but it’s currently up to individual institutions to develop their own management strategies, according to a presentation given April 13 at ARRS 2026.
In his talk, Derek Nguyen, MD, from Duke University in Durham, NC, shared insights on surveillance imaging strategies and modalities after breast cancer treatment for institutions.
“To them [women], hopefully the nightmare is over and they proceed to living a life without cancer,” Nguyen said. “But when we get to this stage, there’s questions we’re all thinking about with post-treatment surveillance.”
Women with a personal history of breast cancer have about seven times higher odds of developing a recurrence in their lifetime and four times increased risk of developing an interval cancer.
The three questions that Nguyen said radiologists should ask themselves when going with a surveillance imaging strategy: should patients undergo screening or diagnostic imaging, how long should they undergo surveillance for, and what supplemental imaging method should be used?
Screening or diagnostic imaging?
While imaging societies recommend annual mammography for these women, they don’t specify whether this should be performed in a screening or diagnostic setting. And evidence is mixed on which is better. Nguyen said it’s up to institutions to determine this.
While screening mammography saves on costs for women and is accessible, it may lead to higher recall rates and patient anxiety. Diagnostic imaging leads to same-day evaluation of abnormalities and real-time interpretation. However, it adds to out-of-pocket costs for patients. And some diagnostic tools may not be as accessible as a mammogram.
“We need the tools. We need the ability to potentially do an ultrasound or potentially do a biopsy. And for a lot of institutions, this may not be available on site,” Nguyen said. “So, that kind of leads to another access disparity if we’re doing diagnostics.”
Nguyen and colleagues led a study published in 2021, which found that about 70% of U.S. institutions opt for diagnostic imaging in some form for breast surveillance. Nguyen also said his team at Duke University does two years of diagnostic imaging follow-up after breast conservation surgery with contrast-enhanced mammography (CEM).
How long and how frequent?
The same 2021 study by Nguyen et al says most women return to screening after either two to three years or four to five years of diagnostic mammography workup.
A 2016 study that Nguyen cited analyzed annual hazard rates of recurrence in breast cancer survivors. The researchers found that the hazard of recurrence was highest during the first five years (10.4%), with a peak between years one and two (15.2%).
“It makes sense that the majority of institutions are doing this two-to-three-year diagnostic follow-up,” Nguyen said. “They’re trying to catch this peak as to when these patients may likely recur.”
While radiologists look for masses, asymmetries, distortions, and calcifications during surveillance, Nguyen said they should look at the original cancer for clues. The available evidence suggests that most recurrences appear as calcifications.
“If it’s calcifications, then have a heightened sense when you’re looking at that lumpectomy site,” he said.
Prior research also suggests that coarse calcifications are mostly noncancerous, but if they’re associated with suspicious calcifications (fine pleomorphic, fine linear, etc.), they may indicate recurrence.
“You have to be sure that whenever you look at the next six-month follow-up, if these calcifications change to any different morphology that is not coarse, you intervene and you biopsy them,” Nguyen said.
Derek Nguyen, MD, shares his thoughts about choosing the best surveillance breast imaging strategies that don't burden patients.
Too long of a duration meanwhile may discourage some women from adhering to surveillance strategies. This may be due to higher costs for diagnostic imaging and less accessibility to some surveillance imaging methods.
“About 70% will come to the first one [appointment], but after that, the adherence drops off dramatically,” Nguyen said.
The evidence is mixed on whether women should be imaged every six months or annually. This is institution dependent. Nguyen said the Duke team employs annual diagnostic follow-up for these women and found no significant differences between annual and twice-annual follow-up.
Which supplemental imaging method?
Ultrasound, MRI, and CEM are the main supplemental imaging modalities considered for surveillance strategies for breast cancer survivors.
While ultrasound uses no radiation and is cost-effective, it does not help detect more cancers in women with a history of breast cancer.
However, imaging societies recommend that women younger than 50 years undergo MRI. MRI leads to over 15 additional cancers found per 1,000 women, according to prior research, and uses no radiation. However, barriers such as lack of accessibility, higher costs, and tolerability limit its use.
CEM meanwhile has emerged as a potential alternative to MRI, with recent studies suggesting that it can detect nearly as many cancers as MRI and is better tolerated by women. CEM may also be more cost-effective for women.
However, there is no official recommendation on CEM use. The modality is also limited by patient positioning, implementation challenges, and the risk of contrast reactions.
“It [CEM] potentially could be an option, but right now it’s not fully yet,” Nguyen said.