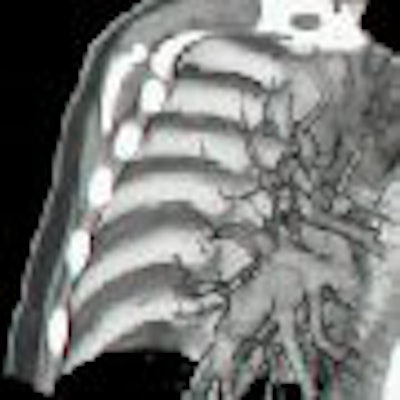
Three-dimensional CT images are more than just pretty pictures when it comes to cardiothoracic surgery. Viewing 3D real-time images along with 2D ones can alter surgical plans for complex cases, and even increase a surgeon's confidence in the plan, according to a new study by researchers from the University of North Carolina (UNC) at Chapel Hill and the University of Alabama at Birmingham.
The study assessed the usefulness of 3D visualization using the SeeThru real-time 3D volume-rendering application developed at UNC on 23 complex cardiothoracic cases. The cases were of six types: heart-lung and lung transplantation, tumor resection, airway stent placement, congenital heart defect repair, aortic aneurysm repair, and resection of pulmonary arteriovenous malformation.
The cases were evaluated first with a standard tiled 2D slice presentation, and later with the SeeThru interactive tool. The 2D images were reviewed with the standard clinical procedure: first by the radiologist and later by the surgeon and radiologist on the body CT alternator viewbox. After the initial opinion was decided, both reviewed the 3D images, and individually assessed the benefits of using them in addition to the 2D images.
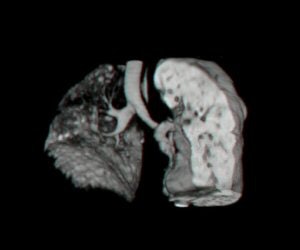 |
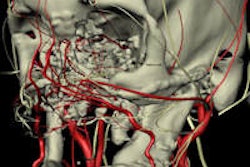
| Above: View of the airways of the lungs for living lung donor transplant case. Used to decide which portion of lung on right or left to take from donor. Below: View of the vascular structure of the lungs for living lung donor transplant case. Used to decide which portion of lung on right or left to take from donor. All images courtesy of Dr. Bradley M. Hemminger. |
 |
The researchers found that 3D visualization changed the surgical plan in 65% of cases, and increased the surgeon's confidence by 40% per case on average.
Radiologists reported new findings or additional information about existing findings in 66% of the cases, and changed their report in 13%. "Although the radiologists reported fewer and less major changes than the surgeons in their understanding of the case due to the 3D visualization, the changes were still statistically significant," the researchers wrote in their study published in the Journal of Digital Imaging (June 2005, Vol. 18:2, pp. 145-153).
How beneficial is 3D visualization?
Among the 23 cases evaluated, radiology reports were changed in three and the surgical plan changed in eight after the second viewing with 3D. Fifteen of the 27 findings were seen better with 3D visualization, and three were seen exclusively with it. None of the findings were worse with 3D imaging, although there was no difference between 3D and film in nine cases. There was also no difference in the radiologist understanding of the case in nine cases.
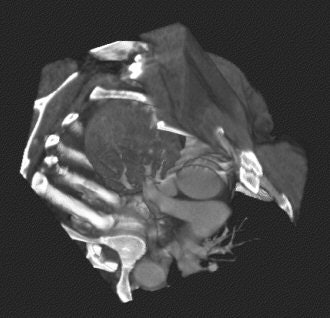 |
| Dramatic example of a large lung mass that was initially deemed inoperable. After use of 3D visualization, surgeons decided there was a possible way to operate. Operation was a success, and patient survived. |
After 3D viewing, radiologists said their understanding was "slightly better" in 10 cases and "moderately better" in four cases, but not "significantly better" in any of the cases (95% CI). On the other hand, 3D visualization helped the radiologist convey the information to the surgeon "significantly better" in four cases, "moderately better" in eight cases, and "slightly better" in seven cases. In four cases there was no difference between 3D and film when it came to conveying the information to the surgeon.
The surgeon's confidence in the surgical plan improved with the 3D visualization in all 23 cases. According to the participating surgeons, 3D visualization made the surgical plan "significantly better" in eight cases and "slightly better" in 10 cases. There was no difference in one case. The surgeons also reported that the correlation between the anatomy seen on 3D imaging and the anatomy seen on surgery was a "moderately good match" for four cases (21%) and a "very good match" for 14 (74%).
"Nonradiologist medical staff seemed to benefit significantly from the 3D presentation," the researchers wrote. 3D visualization also supported discussion of diagnosis and surgical procedure planning, facilitating group consensus while viewing and manipulating the model of the anatomy, the group stated. In one instance following 3D visualization, the surgeon decided to use a Silastic instead of a wire stent.
And in one instance in which the radiologist report was changed, the 3D visualization demonstrated narrowing of the origin of the left carotid artery, which was not shown on 2D images.
3D visualization
"The real-time 3D visualizations and interactive 2D multiplanar reformat (MPR) views that were utilized by SeeThru in this study are now available on most major commercial systems supporting opacity-based 3D real-time or near real-time volume rendering, including such products as GE Advantage Windows, Siemens Virtuoso, Vital Images Vitrea, and Voxar PlugNView 3D," the authors wrote.
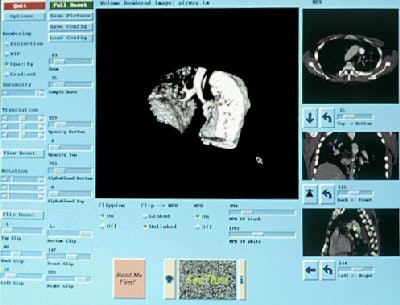 |
| The SeeThru user interface used for combined 2D/3D presentation for both diagnostic readings and therapy planning. MPR (2D) views are on the right side; in the center is the 3D visualization. All parameters and display controls act in real time, so that any change updates the visualization in 1/10th of a second. |
The scans were acquired in a single breath-hold at the thinnest slice thickness that covered the required area without increasing the normal radiation dose on a Somatom Plus spiral CT (Siemens Medical Solutions, Malvern, PA). The datasets were reconstructed using the standard Siemens' reconstruction algorithms in slices spaced at approximately half the acquisition thickness of 8 mm, 5 mm, or 3 mm. The images were sent electronically to the 3D workstation where they were visualized using SeeThru.
The studies were acquired in 512 x 512 pixels of up to 64 slices, creating a 512 x 512 x 64 volume. "An opacity-based direct volume-rendering algorithm was used which did not incorporate gradient information and had a fixed light source," the authors wrote.
3D visualization has a positive effect in cardiothoracic surgery planning, which is a difficult visualization problem because of the small contrast differences in the soft tissue to soft-tissue boundaries, the authors noted.
They suggested that from a practical standpoint, surgeons should have 3D visualization capabilities on their primary workstation, and radiologists should have convenient access to their PACS, or a nearby workstation.
By N. Shivapriya
AuntMinnie.com contributing writer
June 13, 2005
Related Reading
3D diagnosis and planning bring orthodontists closer to 'anatomic truth,' June 2, 2005
3D: Rendering a new era, May 2, 2005
3D and the future of imaging, November 3, 2003
Copyright © 2005 AuntMinnie.com