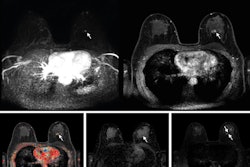
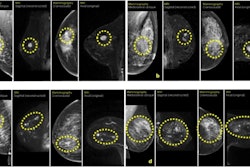
Abbreviated MRI may be suitable for screening women with dense breasts, a study published May 22 in the American Journal of Roentgenology found.
Researchers led by Christine Edmonds, MD, from the University of Pennsylvania in Philadelphia, found that subsequent rounds of abbreviated breast MRI screening in patients with dense breasts had lower abnormal interpretation rates compared with baseline examinations. Meanwhile, high cancer detection rates were also maintained.
"Radiologists and ordering clinicians, alike, may use these results as evidence of the value of abbreviated MRI beyond the first round of screening in this population," Edmonds told AuntMinnie.com.
Previous studies have demonstrated abbreviated breast MRI’s performance in high cancer detection rates when applied for baseline supplemental screening in women with dense breasts. However, the researchers noted that limited data is available on the modality’s performance in subsequent screening rounds.
Edmonds and colleagues compared outcomes between baseline and subsequent rounds of screening abbreviated MRI in women with dense breasts. The women otherwise had an average risk of developing breast cancer.
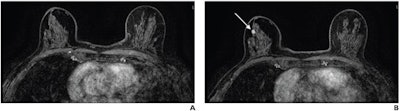 (A) Axial subtracted contrast-enhanced fat-suppressed T1-weighted image from a baseline abbreviated MRI examination is negative (BI-RADS category 1). (B) Axial subtracted contrast-enhanced fat-suppressed T1-weighted image from a subsequent-round abbreviated MRI examination performed two years later shows a new 5-mm enhancing mass in the upper outer right breast (arrow), which was not seen on a mammogram performed five months prior. The exam was assessed as BI-RADS category 5. Ultrasound-guided core biopsy yielded invasive ductal carcinoma (ER+/PR+/HER2-). Image courtesy of the ARRS.
(A) Axial subtracted contrast-enhanced fat-suppressed T1-weighted image from a baseline abbreviated MRI examination is negative (BI-RADS category 1). (B) Axial subtracted contrast-enhanced fat-suppressed T1-weighted image from a subsequent-round abbreviated MRI examination performed two years later shows a new 5-mm enhancing mass in the upper outer right breast (arrow), which was not seen on a mammogram performed five months prior. The exam was assessed as BI-RADS category 5. Ultrasound-guided core biopsy yielded invasive ductal carcinoma (ER+/PR+/HER2-). Image courtesy of the ARRS.
The retrospective study included data collected between 2016 and 2023 for 2,585 abbreviated MRI exams. Of the total, 2,007 were baseline exams while 578 were subsequent-round exams. The exams were performed for supplemental screening in 2,007 women with dense breasts with an average age of 57.1 years.
Among baseline exams, 1,658 (82.6%) were categorized as BI-RADS 1 or 2, 171 (8.5%) were BI-RADS 3, and 178 (8.9%) were BI-RADS 4 or 5. For subsequent-round exams, 533 (92.2%) were BI-RADS 1 or 2, 20 (3.5%) were BI-RADS 3, and 25 (4.3%) were BI-RADS 4 or 5 (p < 0.001).
The researchers also reported a higher abnormal interpretation rate among baseline exams compared to subsequent-round exams, as well as comparable positive predictive values and cancer detection rates between the two exam types.
| Comparison between baseline, subsequent-round screening with abbreviated MRI | |||
|---|---|---|---|
| Measure |
Baseline |
Subsequent round |
p-value |
| Abnormal interpretation rate |
17.4% |
7.8% |
< 0.001 |
| Cancer detection rate | 18.9 per 1,000 exams |
12.1 per 1,000 exams |
0.37 |
| PPV2 |
21.3% |
28% |
0.45 |
| PPV3 |
26.6% |
29.2% |
0.81 |
Edmonds and colleagues found that all 45 cancers diagnosed by baseline or subsequent-round abbreviated MRI were stage 0 or 1. Seven cancers diagnosed by subsequent-round abbreviated MRI had the following characteristics: an average interval since prior examination of 872 days, size of 0.3 to 1.2 cm, and node-negative status at surgical axillary evaluation.
The group highlighted that the study results support the use of abbreviated MRI for both baseline and subsequent screening rounds in women with dense breasts.
Edmonds told AuntMinnie.com that the team hopes to conduct subsequent investigations to optimize the abbreviated MRI screening interval and to compare the accuracy of abbreviated MRI to routine, full-protocol breast MRI for supplemental screening of women with dense breasts. She said that this could identify more cost-effective, accessible screening strategies.
The study can be found in its entirety here.