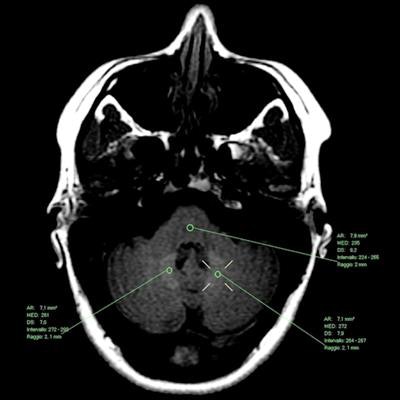
Seeing is believing for Italian researchers who used MRI to visually confirm evidence of gadolinium retention in patients with multiple sclerosis (MS) and who had undergone several MRI scans with a gadolinium-based contrast agent (GBCA). The findings were published September 4 in Insights into Imaging.
The researchers noted increased T1-weighted signal intensity in patients who had received the GBCA. Also, effects from gadobutrol (Gadavist, Bayer) and gadoterate meglumine (Dotarem, Guerbet) appeared to depend on the number of administrations, with T1 hyperintensity most evident after the fourth or fifth GBCA-enhanced scan.
But the researchers also found no evidence that the visible T1 hyperintensities or increases in signal intensity ratios in the dentate nucleus/pons region of the brain had any adverse effect on patient health or safety.
"The results of our study provide clear evidence that T1 signal changes can and do occur in the dentate nucleus after multiple administrations of the macrocyclic GBCAs gadobutrol and gadoterate meglumine, and that the appearance of visible T1 hyperintensity is associated with significant increases in dentate nucleus/pons signal intensity ratio," wrote lead author Dr. Alessandra Splendiani and colleagues at the University of L'Aquila.
The use of GBCA-enhanced MRI scans is a particularly pesky issue for patients with relapsing-remitting MS who undergo multiple exams to detect new inflammatory lesions that could indicate disease activity or progression. Previous research on T1 signal changes in the dentate nucleus and/or global pallidus of these patients after multiple administrations of macrocyclic GBCAs have yielded "conflicting results," the authors noted. While some studies have found no T1 signal changes at all, other results have recorded "marked quantitative changes."
To further investigate, Splendiani and colleagues viewed results from 149 patients with confirmed relapsing-remitting MS who underwent two or more 3-tesla MRI scans (Signa Excite, GE Healthcare). The scanning protocol included axial T1-weighted spin-echo, T2-weighted, and susceptibility-weighted imaging sequences before and after GBCA injection. Among the subjects, 63 patients (42%) received gadobutrol, 57 patients (38%) were given gadoterate meglumine, and 29 patients (19%) received both GBCAs.
In comparing T1 hyperintensity before and after MRI scans, 42 patients (28%) showed statistically significant differences in mean dentate nucleus/pons signal intensity ratio for the individual GBCAs and when patients received both contrast agents.
| Mean dentate nucleus/pons signal intensity ratios in patients with T1 hyperintensity | ||||
| No. of patients | Before 1st scan | Before last exam | p-value* | |
| Gadobutrol | 19 | 0.998 | 1.153 | < 0.0001 |
| Gadoterate | 15 | 1.003 | 1.110 | < 0.0001 |
| Both GBCAs | 8 | 1.004 | 1.163 | < 0.0004 |
| Total | 42 | 1.003 | 1.137 | < 0.0001 |
"Typically, the first appearance of visible T1 hyperintensity in positive patients occurred at the fourth or fifth follow-up exam, [and] between approximately three and four years after the initial MRI examination," the authors wrote.
The number of GBCA administrations also influenced signs of visible T1 hyperintensity, with 43 patients (40%) who received five or fewer doses of the study's GBCAs showing no evidence of visible T1 hyperintensity, compared with seven patients (17%) with visible T1 hyperintensity.
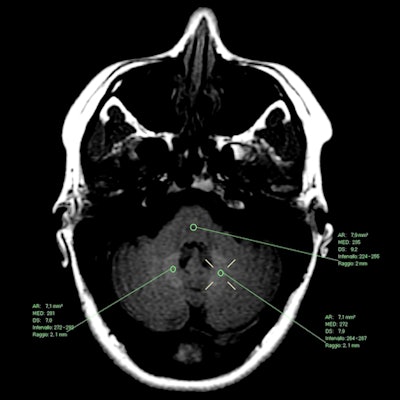 MR image from a 36-year-old female patient who received seven administrations of gadoterate meglumine. The mean dentate nucleus/pons ratio on T1-weighted spin echo increased from 1.09 at the first scan in July 2006 to 1.18 at her last scan in February 2010. Images courtesy of Splendiani et al and Insights into Imaging.
MR image from a 36-year-old female patient who received seven administrations of gadoterate meglumine. The mean dentate nucleus/pons ratio on T1-weighted spin echo increased from 1.09 at the first scan in July 2006 to 1.18 at her last scan in February 2010. Images courtesy of Splendiani et al and Insights into Imaging."The strength of our study lies in the fact that all patients received only macrocyclic GBCAs and that imaging was performed in a carefully monitored manner exclusively at our center. Therefore, the possibility that patients with visible T1 hyperintensity could have received prior administrations of certain linear GBCAs that are more widely associated with T1 signal changes in the dentate nucleus can be excluded," Splendiani and colleagues concluded.