Given its high diagnostic accuracy without the use of contrast and its lack of ionizing radiation, MRI should be elevated to a first-line imaging test for patients younger than 50 who come to the emergency department (ED) with suspected acute appendicitis, according to a study published in the May issue of Radiology.
Researchers from the University of Arizona also found MRI quite proficient at assessing secondary causes of abdominal pain, providing images that allowed readers with various levels of training to achieve high levels of diagnostic accuracy (Radiology, May 2016, Vol. 279:2, pp. 451-460).
"MRI can be used to comprehensively evaluate abdominal and pelvic soft tissues without ionizing radiation, and it may be performed without use of intravenous or oral contrast material," wrote lead author Dr. Iva Petkovska and colleagues. "Consistent high levels of accuracy were seen across readers with disparate levels of training, including interpretations performed by overnight residents."
Common occurrence
Acute appendicitis is a common cause of acute pain in the lower right side of the body. Healthcare providers in the ED generally use ultrasound or CT initially to diagnose the problem and to determine if surgery is necessary. They are more inclined to choose MRI for pregnant women and children to avoid exposing these more vulnerable patients to radiation and the use of contrast, according to the authors.
Previous papers have noted excellent diagnostic results with MRI for appendicitis evaluation in all patient groups; however, there has been little research to determine MRI's performance when used as the initial imaging test for acute right lower body pain in a general ED population, Petkovska and colleagues wrote.
The University of Arizona initiated a protocol developed by the medical imaging department and the ED to perform unenhanced, accelerated MRI as the initial scan for patients younger than 50 years who are suspected of having acute appendicitis.
Not only does this strategy save patients from radiation and contrast, but the "approach provides potential time savings, which is an important consideration in the setting of emergency care," the authors wrote.
To evaluate the effect of the MRI-first protocol, the researchers performed a retrospective study that analyzed 403 patients (mean age, 21 years; range, 3-49 years) who came to the ED with pain in the abdomen between August 2012 and July 2014.
All MRI exams were conducted on a 1.5- or 3-tesla scanner (Magnetom Aera or Magnetom Skyra, Siemens Healthineers) with two 18-channel torso phased-array anterior coils and a 32-channel table-integrated posterior coil to enhance signal reception.
Eight attending physicians and 26 residents read MR images in real-time over the course of the two-year study. All of the readers had access to the patients' clinical information, as the scan was part of each diagnostic workup. Their findings were classified according to five categories, ranging from "definitely acute appendicitis" to "definitely not acute appendicitis."
Surgical and histopathologic results served as the reference standard to confirm a diagnosis of acute appendicitis for patients who underwent surgery. The reference standard for patients who did not go under the knife was a minimum eight-week clinical follow-up by phone or a medical record review six months after their MRI.
Diagnostic accuracy
In all, 77 patients went on to the operating room after MRI, based on the scans or other factors such as persistent clinical symptoms. Surgery confirmed 67 cases of acute appendicitis, and of these patients, 65 (97%) had positive MRI results. Among the 10 patients who were negative for appendicitis at surgery, eight (80%) had negative MRI results.
Meanwhile, among the 326 patients not sent to surgery, the researchers were able to determine outcomes for 291 patients. None of those individuals were found to have developed acute appendicitis.
When compared with surgery and clinical follow-up, MRI achieved an overall sensitivity of 97% and specificity of 99%, according to the authors. Positive predictive value was 97% and negative predictive value was 99%.
"MR imaging showed excellent results for the diagnosis of acute appendicitis when compared with surgical results and clinical follow-up," they wrote.
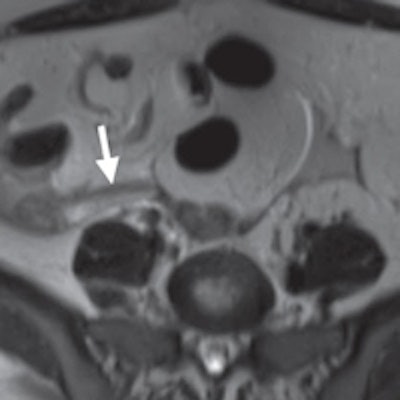
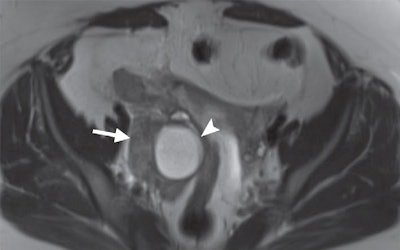 MRI of a 31-year-old woman with a ruptured hemorrhagic ovarian cyst and false-positive interpretation for acute appendicitis. Axial single-shot T2-weighted image shows a right ovarian cyst (above, arrowhead) with complex material along the lateral margin of the cyst (arrow). In retrospect, axial single-shot T2-weighted MRI shows a nonfluid-filled appendix (below, arrow) and no inflammation in the periappendiceal soft tissues. The patient underwent subsequent surgery. Images courtesy of Radiology.
MRI of a 31-year-old woman with a ruptured hemorrhagic ovarian cyst and false-positive interpretation for acute appendicitis. Axial single-shot T2-weighted image shows a right ovarian cyst (above, arrowhead) with complex material along the lateral margin of the cyst (arrow). In retrospect, axial single-shot T2-weighted MRI shows a nonfluid-filled appendix (below, arrow) and no inflammation in the periappendiceal soft tissues. The patient underwent subsequent surgery. Images courtesy of Radiology.When Petkovska and colleagues analyzed the results by reader type, they found that attending physicians were slightly more accurate than radiology residents in their preliminary overnight MRI interpretations. However, the difference was not significant.
"Consistent high levels of accuracy were seen across readers with disparate levels of training, including interpretations performed by overnight residents," they wrote.
The researchers credited a shortened fast-acquisition MRI technique based on a single-shot spin-echo method that is relatively insensitive to motion for the similarly high accuracy of interpretations between the residents and more experienced physicians.
Despite its clinical benefits, the relatively high cost of MRI is often a deterrent to its use in certain settings, the authors acknowledged. They recommended a detailed analysis using MR imaging as a first option in suspected appendicitis cases to evaluate costs and outcomes.