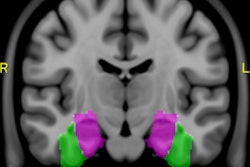
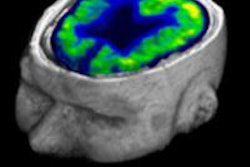
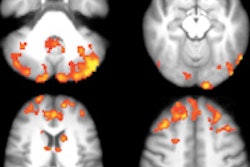
Functional MRI (fMRI) can inspire new treatment and rehabilitation protocols based on the neuronal plasticity and redistribution of the cortical representation of a function, but to accurately describe the location of lesions in their reports, it's vital radiologists recognize anatomical landmarks, noted award-winning Spanish researchers at ECR 2016.
Introduction of fMRI in clinical practice adds value to the correlation of imaging with patients' symptoms and signs, and it can help establish treatment plans, noted lead author Dr. Iván Camilo García Duitama, from the department of radiology at Bellvitge University Hospital, a public hospital in Barcelona, Spain.
His group's e-poster, "Functional MR of the brain: ABC for Beginners. It's a good moment to review functional anatomy," received a cum laude award at the congress in Vienna, which ended on Sunday.
Radiologists need to understand the topographic functional anatomy of the brain, keep aware of the location of a lesion based on its clinical manifestations and vice versa, know about the principles of fMRI, and choose the functional paradigm according to the location of a lesion. They must be able to interpret real-life cases and understand the clinical transcendence of fMRI and implications for patient care, García Duitama and colleagues stated.
"More recently with the arrival of medical imaging methods such as single photon emission CT, PET/CT and functional fMRI, we have a more physiologically based understanding of cerebral complexity. fMRI combines high anatomical resolution with information about cortical activation to obtain detailed maps of the specific areas involved in a given task," they wrote. "A theoretical brain functional map allows the radiologist to plan the fMRI and interpret its results correctly."
The human brain can perform a wide variety of tasks, but in clinical practice, it's necessary to evaluate the most elemental forms of cortical activity: motor, somatosensory, verbal, visual, and auditory.
Key principles of functional MRI
Functional MRI is based on the blood-oxygen-level dependent (BOLD) effect occurring during neuronal stimulation. The nervous system is deeply related to the vascular system, which can adapt to the brain's need for oxygen and other substrates, the so-called neurovascular coupling, the authors explained. Neuronal activity produces an increase in the tissue's oxygen demands, which is supplied through neurovascular coupling. This in turn elevates the regional arterial blood flow for a period of seconds to maintain oxyhemoglobin levels higher than the deoxyhemoglobin ones, leading to a net increase in oxyhemoglobin concentration, or, in other words, a decrease in deoxyhemoglobin concentration.
"The greater the area of cortical activation is, the more the time it takes to the vascular system to adapt itself for supplying arterial blood flow to these activated areas," they added. "fMRI displays a vascular process as an indirect marker of brain activity, which in turn can be a little imprecise."
In clinical practice, the most extended indication is the presurgical mapping of the cortex in patients with brain tumors or vascular malformations located in eloquent areas and epilepsy refractory to the conventional treatment, mainly on the temporal lobe. There are three goals in the presurgical assessment: determine the risk of neurological deficit after the surgery, select patients for intraoperative mapping, and guide the surgery itself.
Even in healthy individuals, the cortical representation of a function may vary, making the conventional MRI scan incomplete. On the other hand, the effect of lesions in adjacent tissues can lead to the loss of anatomical landmarks or change the normal cortical distribution of functions. A distance on fMRI of 10 mm or more between the tumor and the functional cortex reduces the risk of postoperative loss of function.
Furthermore, overlapping of a lesion with eloquent areas may exist, and a surgical plan should be made to perform the maximum safe partial resection or a conservative treatment (i.e., chemotherapy, radiotherapy, or Gamma Knife ablation). In these latter cases, intraoperative mapping is mandatory due to the slight imprecision of the fMRI exam, according to the group. Also, fMRI can demonstrate activations on areas related to but not absolutely necessary for a given task and could therefore be resected without significant sequels. Intraoperative mapping makes it possible to determine which of these secondary areas are crucial for the task.
"Particularly when assessing the language function, an intraoperative electrocortical stimulation has to be done, but even in those cases fMRI is a valuable tool for planning the surgery and mapping eloquent areas, because it can reduce the extent of the craniotomy and, thus, the duration of the intervention," they pointed out.
Diffusion tensor imaging
Diffusion tensor imaging (DTI) fiber tracking is a relatively new MR technique that demonstrates the orientation and integrity of the white-matter tracts, including corticospinal and corticobulbar tracts, arcuate fasciculus, corpus callosum, and cerebellar peduncles, the authors continued.
DTI fiber tracking is commonly performed after the fMRI exam but during the same MRI session. In this way, the fiber tract associated with a cortical activation can be demonstrated and, thus, corroborates its eloquent meaning instead of an artifact signal. Knowing the distribution of the fiber tracts is an aim to interpret the cases in which an odd distribution of the cortical activation is observed -- e.g., language testing shows a great variation of cortical activation among subjects, but the conjunction of activation and subcortical language tracts helps ensure that the hypersignal doesn't correspond to an artifact. DTI also permits the assessment the effect of a tumor or peritumoral edema in a specific tract.
To view the ECR 2016 e-poster in full, click here.