By using functional MRI (fMRI) to view regions of the brain that play a role in regulating consciousness, French researchers may have discovered a way to predict which patients could emerge from a coma.
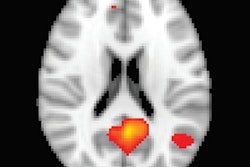
The study, published online November 11 in Neurology, showed significant disruptions in the connections between certain brain regions and the posterior cingulate cortex among comatose subjects compared to healthy controls.
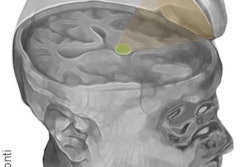
In addition, brain activity between the posterior cingulate cortex, which is strongly associated with cognitive function, and the medial prefrontal cortex differed significantly between patients who eventually recovered from their comas and those who remained in a minimally conscious or vegetative state.
Lead author Dr. Stein Silva, PhD, from the French Institute of Health and Medical Research in Toulouse, and colleagues noted similar patterns between the posterior cingulate cortex and medial prefrontal cortex in healthy subjects and patients who regained consciousness.
The researchers compared 27 comatose patients who had severe brain injuries with 14 age-matched healthy individuals. The imaging protocol included 11 minutes of resting-state fMRI on a 3-tesla scanner (Intera Achieva, Philips Healthcare).
Standardized clinical assessment and fMRI scans were performed an average of four days after sedative drugs were out of the comatose patients' systems. The researchers focused on the posteromedial cortex area for the fMRI scans, based on recent studies that suggest this region plays a major role in regulating consciousness.
Follow-up revealed that four comatose patients regained consciousness three months after their injuries, while the other patients remained in a minimally conscious or vegetative state. Silva and colleagues traced the clinical difference between the recovered patients and those still in a coma to the significant difference in functional connectivity strength between the posterior cingulate cortex and medial prefrontal cortex at the acute stage of the coma when the subjects were scanned.
"Of note, we found that acute brain injuries responsible for coma yield a reorganization of existing intrinsic brain networks rather than a complete annihilation," which may partly explain the four recoveries, according to the authors.
They emphasized that additional research is needed to validate the results.