PET/CT imaging has shown for the first time in a clinical trial that aortic inflammation is reduced in lymphoma patients after first-line chemotherapy, according to a study published March 31 in JACC: Advances.
The finding may have important implications for tracking the risk of cardiovascular diseases in patients undergoing treatment and should prompt further research, noted first author Dr. Charalambos Vlachopoulos, of the National and Kapodistrian University of Athens in Greece, and colleagues.
"Whether these findings are associated with the type of treatment or with individual patient response to treatment needs to be investigated," the group wrote.
Despite significant advances in the treatment of oncology patients, therapy-related side effects can lead to premature morbidity and death among survivors, Vlachopoulos and colleagues noted. Concerns for these patients and potential side effects are mainly regarding accelerated development of cardiovascular disease (CVD) or even direct effects of treatment on the heart muscle.
Yet despite intensive research on the heart itself, there is little evidence of the effect of chemotherapy on larger arteries and peripheral vasculature, the researchers explained.
The team conducted a clinical trial in 65 patients with Hodgkin or non-Hodgkin lymphoma using F-18 FDG-PET/CT imaging, a tool with an established role in staging lymphomas. Importantly, both cancers originate in the lymphatic system, but different lymphatic cells drive the diseases.
Thirty-three patients had a confirmed diagnosis of Hodgkin lymphoma and 32 with a diagnosis of non-Hodgkin lymphoma. All underwent PET/CT imaging between July 2015 and July 2019; studies were taken at baseline, at an interim phase, and after first-line treatment. At each phase, the investigators assessed aortic uptake of the FDG radiotracer by measuring global aortic target-to-background ratio and serum biomarkers for inflammation (interleukin-6 and interleukin-1b).
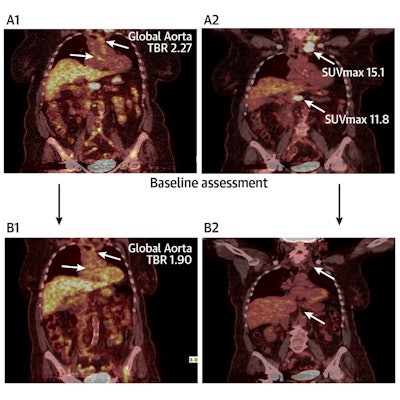
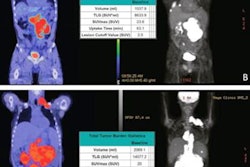
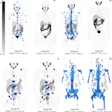
 Central illustration: Aortic inflammation as assessed by F-18 FDG-PET-CT is reduced in Hodgkin lymphoma patients after first-line treatment, but not in non-Hodgkin lymphoma. Image and caption courtesy of JACC: Advances through CC BY 4.0.
Central illustration: Aortic inflammation as assessed by F-18 FDG-PET-CT is reduced in Hodgkin lymphoma patients after first-line treatment, but not in non-Hodgkin lymphoma. Image and caption courtesy of JACC: Advances through CC BY 4.0.The study showed that patients with Hodgkin lymphoma demonstrated a significant reduction in aortic target-to-background ratio after first-line treatment, which remained significant after the researchers adjusted for confounders. In contrast, patients with non-Hodgkin lymphoma did not demonstrate a significant aortic inflammation response.
In addition, patients with Hodgkin lymphoma demonstrated a significant reduction in interleukin-6 (IL-6) and interleukin-1b (IL-1b), whereas patients with non-Hodgkin lymphoma did not demonstrate significant reduction in IL-6 and IL-1b levels.
"These findings imply that different pathophysiological pathways and different therapies might affect the arterial bed in different ways for patients with lymphoma," the group explained.
While the results may point toward specific pathophysiological differences between Hodgkin lymphoma and non-Hodgkin lymphoma, they cannot prove causality, the investigators cautioned. Larger prospective multicenter studies are needed.
Given that traditional CVD risk scores typically underperform in cancer patients, incorporating tools such as PET/CT aortic FDG uptake may improve risk prediction in this population, wrote Dr. Arielle Abovich and Dr. Roberta Florido of Johns Hopkins University in Baltimore in an accompanying editorial.
"Studies with a longer follow-up period would be useful to determine if lack of decrease in aortic inflammation after treatment correlates with increased CVD risk," Abovich and Florido concluded.










![A 53-year-old patient (patient number four) with a recurrent pituitary adenoma with extension of a cystic component of disease to the medial temporal lobe apparent on MRI (contoured in blue), and extension of disease to the left sphenoid bone and orbital apex apparent on [68Ga]Ga-DOTA-TATE (contoured in yellow).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/04/pituitary-tumor.QGsEnyB4bU.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)