Dynamic chest radiography has demonstrated potential as a less-invasive tool than right heart catheterization for assessing hemodynamics in patients with heart failure, according to research published February 4 in the European Journal of Radiology.
Researchers led by Dr. Hiroaki Hiraiwa, PhD, of Nagoya University Graduate School of Medicine in Nagoya, Japan compared the two methods in a group of patients. They found that dynamic chest x-ray digital metrics correlated strongly with blood flow measurements acquired during invasive catheterization procedures. Given that dynamic chest radiography is noninvasive, the emerging modality holds promise for improving patient care, according to the group.
"Dynamic chest radiography demonstrates potential as a less invasive tool than right heart catheterization and is convenient for hemodynamic assessment in heart failure," the group wrote.
Hemodynamic assessment is essential for heart failure monitoring, with heart catheterization procedures as the gold standard for assessments. However, these are invasive and associated with complications, according to the authors.
Conversely, dynamic chest radiography is a novel, minimally invasive, and comparatively low-cost technique that has shown promise in previous studies visualizing cardiac and pulmonary blood flow expressed in pixel values, they wrote. They believe these values may correlate with standard hemodynamic parameters, yet data on the use of the modality for this purpose are scarce.
Thus, the researchers aimed to determine whether parameters measured by dynamic chest radiography provide clinical value compared with measurements derived during catheterizations.
The group recruited 20 patients (median age, 67 years; 17 men) hospitalized for worsening heart failure who underwent both procedures at their hospital between March 2022 and July 2022. The dynamic chest radiography images required seven seconds of breath holding, with an average imaging time of 16 seconds and average radiation dose of 1.8 mGy.
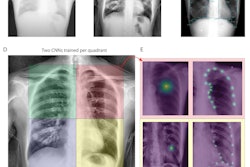
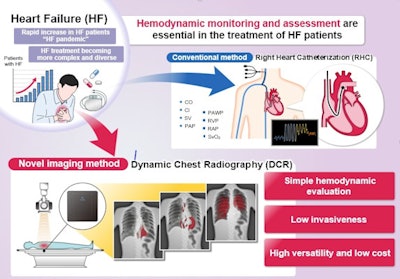 A graphical abstract. Hemodynamic assessment is essential for heart failure monitoring and assessment; however, it is invasive and is associated with complications. Dynamic chest x-ray (DCR) is a novel, minimally invasive, low-cost, and versatile imaging modality that can be used to visualize cardiac and pulmonary blood flow as pixel values, which correlate with hemodynamic parameters. Thus, DCR may be a useful alternative to estimate hemodynamic parameters in patients with HF. Image and caption courtesy of the European Journal of Radiology through CC BY 4.0.
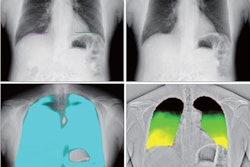
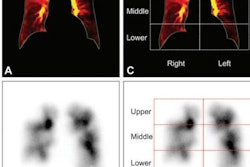
A graphical abstract. Hemodynamic assessment is essential for heart failure monitoring and assessment; however, it is invasive and is associated with complications. Dynamic chest x-ray (DCR) is a novel, minimally invasive, low-cost, and versatile imaging modality that can be used to visualize cardiac and pulmonary blood flow as pixel values, which correlate with hemodynamic parameters. Thus, DCR may be a useful alternative to estimate hemodynamic parameters in patients with HF. Image and caption courtesy of the European Journal of Radiology through CC BY 4.0.First, the researchers calculated right atrial, right pulmonary artery, and left ventricular apex pixel values in the dynamic chest radiography images. Next, they analyzed correlations between rates of change in these pixel values with right atrial pressure, pulmonary artery pressure, pulmonary artery wedge pressure, and cardiac index findings from the catheterization procedures.
According to the findings, the researchers observed the following correlations:
- Mean right atrial pixel value and mean right atrial pressure (r = -0.576, p = 0.008)
- Mean right pulmonary artery pixel value and mean pulmonary artery pressure (r = -0.546, p = 0.013)
- Left ventricular apex pixel value change rate and mean pulmonary artery wedge pressure (r = -0.664, p = 0.001) or cardiac index (r = 0.606, p = 0.005)
"Overall, we believe that the correlations between hemodynamic parameters and dynamic chest radiography pixel values may be useful to derive predictive models and formulas to estimate cardiac index and pulmonary artery wedge pressure," the researchers wrote.
The authors noted several limitations, namely that the modality is difficult to use in patients with implanted cardiac devices because these devices can affect x-ray transmission, and many patients with severe heart failure and very poor cardiac function have these devices. Thus, it will be necessary to examine whether the technique can be used in these patients, they noted.
Nonetheless, future research is warranted, the group wrote.
"In the future, we would like to investigate the relationship between the cardiothoracic ratio (during inspiration, cardiac systole, or cardiac diastole) and other imaging and hemodynamic parameters," Hiraiwa and colleagues concluded.