Aortic calcification visible on chest x-rays is associated with poorer overall survival in patients following minor lower extremity amputation, researchers have reported.
The finding is from an analysis that included 383 patients who underwent amputation after a preoperative chest x-ray within three months prior to surgery, noted lead author Miska Vuorlaakso, MD, of Tampere University in Tampere, Finland, and colleagues.
“Aortic calcifications on chest radiographs may provide useful prognostic information for clinicians treating patients undergoing lower extremity minor amputation,” the group wrote. The study was published on February 7 in JVS-Vascular Insights.
Aortic calcification (AC) -- the build-up of calcium on the aortic valve -- visible on routine imaging such as chest x-ray or CT scans, has emerged as a novel marker of systemic atherosclerosis, the researchers explained. While the prevalence of ACs has been investigated in various populations, including patients undergoing cardiac surgery and kidney transplant surgery, it has not been studied in patients undergoing limb amputation, they noted.
To bridge the gap, in this study, the researchers assessed the association between the presence and degree of ACs on chest x-rays and overall survival, amputation-free survival, and leg salvage among 383 patients who underwent minor amputation below the ankle level between 2007 and 2020. Patients underwent amputations due to peripheral arterial disease and diabetes-related complications.
All patients had an upright antero-posterior chest x-ray acquired within three months before amputation, which were jointly read by two researchers. They categorized AC into three groups using three classification systems: none or mild (no visible calcification or a single focal calcification measuring < 10 mm), moderate (thick or elongated calcification measuring ≥ 10 mm, or multiple focal calcifications), and severe (circumferential or near-circumferential calcification).
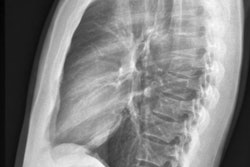
 Grading of radiological findings of aortic calcifications according to the earlier described Symeonidis and Tian classification systems and the novel AV classification system. 1 Symeonidis classification: 0: non-evident, 1: mild, 2: moderate, 3: severe. 2 Tian classification: 0: non-evident, 1: mild, 2: severe. 3 AV classification: 0: non-evident or mild, 1: moderate, 2: severe.JVS-Vascular Insights
Grading of radiological findings of aortic calcifications according to the earlier described Symeonidis and Tian classification systems and the novel AV classification system. 1 Symeonidis classification: 0: non-evident, 1: mild, 2: moderate, 3: severe. 2 Tian classification: 0: non-evident, 1: mild, 2: severe. 3 AV classification: 0: non-evident or mild, 1: moderate, 2: severe.JVS-Vascular Insights
“ACs are commonly detected on chest radiographs of patients undergoing minor amputation, with more than 60% of patients having at least some degree of AC,” the group wrote.
Ultimately, lower limb amputation is an increasingly common major complication of advanced peripheral arterial disease and diabetes mellitus and is associated with decreased quality of life and increased risk of mortality, the authors noted. The high prevalence of ACs among patients undergoing amputation underscores the need to carefully consider atherosclerosis in their management, they wrote.
“The implementation of this simple and widely available marker in clinical decision-making could enhance risk assessment and support the selection of an optimal treatment strategy for patients in limb-threatening situations,” the researchers concluded.
The full study is available here.