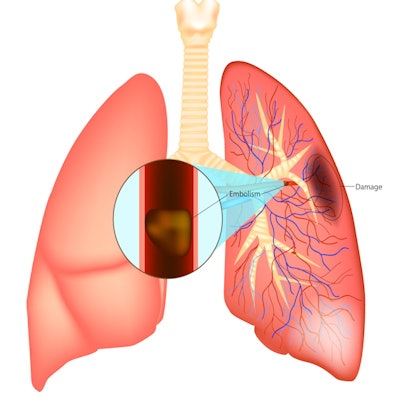
A quarter of patients hospitalized with COVID-19 show pulmonary embolism (PE) on CT pulmonary angiography (CTPA) or nuclear stress testing, according to a study published July 13 in Radiology.
The condition is caused by blocked arteries in the lung, and if untreated, it has a mortality rate of up to 30%, according to a statement released by the RSNA.
A team led by Dr. Sadjad Riyahi of Weill Cornell Medicine in New York City used electronic medical record data from 413 people hospitalized with COVID-19 between March 3 and June 5, 2020. Of these patients, 102 were diagnosed with pulmonary embolism via chest CT or stress testing, and the rate of acute PE was greater in men by 74% and in smokers by 86%. The rate of acute pulmonary embolism did not differ significantly between intensive care and nonintensive care patients, however (29% compared to 24%).
Questions about COVID-19-induced pulmonary embolism and how best to diagnose it remain, wrote Dr. Loren Ketai of the University of New Mexico in Albuquerque in an accompanying editorial.
"While this study confirms several important clinical observations regarding thromboembolism and COVID-19, key practical questions remain unanswered. Not the least important, is how to best identify patients with COVID-19 who will benefit from pulmonary CTPA. ... Even when pulmonary emboli are detected by CTPA or perfusion scintigraphy, their clinical significance in the setting of COVID-19 may be ambiguous," he wrote.