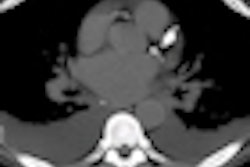
The Houston-based Society for Heart Attack Prevention and Eradication (SHAPE), which wants to scrap population-based cardiac risk assessment in favor of imaging-based evaluation of each individual, said it will release new guidelines at the November American Heart Association meeting in Chicago.
The new SHAPE II guidelines, which will emphasize the utility of 3D ultrasound in carotid intima-media thickness (CIMT) scans, among several other changes, will replace the SHAPE I task force's original 2006 recommendations for coronary artery calcium (CAC) scoring with CT or CIMT for adults between the ages of 45 and 75.
Last year those recommendations led to the organization's biggest legislative coup to date -- passage of the Texas Heart Attack Prevention Bill (HB 1290), which requires healthcare insurers to pay at least $200 every five years toward cardiac risk assessment of middle-aged individuals via CAC or CIMT. After years of delays and setbacks, the controversial Texas law finally went into effect in January.
A new risk-assessment regime
The guidelines now being shaped by the organization's SHAPE II task force will continue to rely on CT-based CAC scoring, as well as ultrasound-based CIMT measurements. However, they will also include 3D evaluation of soft plaque as part of the ultrasound CIMT exam and the use of biomarkers such as C-reactive protein (CRP) in ways that are currently being hammered out in anticipation of their November rollout.
The science of coronary artery risk assessment has progressed significantly since the original guidelines were published in 2006, Morteza Naghavi, MD, SHAPE founder and president, said in an interview with AuntMinnie.com.
"We're arriving at a point where all the evidence is in place clearly showing that noninvasive imaging modalities -- in particular, coronary calcium and carotid IMT -- provide significantly more predictive value for identification of individuals at risk of future events" compared to the Framingham risk score alone, or so-called global assessment that includes a serum cholesterol test, said Naghavi, who is also part of the research firm American Heart Technologies in Houston.
While population-based risk assessment via the Framingham risk score is seen as a good predictor of population-wide risk, it cannot assess an individual's risk of heart disease, Naghavi said.
Nowadays, "we do have methods of measuring atherosclerosis and measuring the severity of atherosclerosis," he said. "You need to treat people with atherosclerosis and you need to titrate the intensity of treatment to the severity of disease," using all of the research results and tools that are now available to evaluate each patient individually, according to Naghavi.
To validate the group's imaging-based approach to risk assessment, SHAPE first approached the National Institutes of Health (NIH) back in 2006, and recently won a commitment to fund a five-year study of atherosclerotic disease risk based on noninvasive imaging.
"We've been able to convince NIH that they should put up enough money to at least do a five-year study," Naghavi said. "We think that the value of a noninvasive approach is so strong it can show the effect even in five years." Securing this study means "we've already accomplished our mission," he added.
The study, to be conducted by NIH's National Heart, Lung, and Blood Institute, will compare the SHAPE approach to the National Cholesterol Education Program (NCEP) of risk assessment, which essentially treats patients who have high low-density lipoprotein (LDL) cholesterol levels, he said. Such an approach is not terribly effective because it doesn't measure coronary plaque, without which the primary adverse event -- myocardial infarction -- simply doesn't occur, he said.
Some have called for a large-scale outcomes study as the only way to properly validate the noninvasive imaging risk-assessment model, but the SHAPE team rejected that option as prohibitively slow and expensive. In any case, Naghavi said, no outcomes studies were conducted on current population-based risk assessment methods before they were implemented, and there are cheaper and more practical ways to validate the new individualized prediction models, he believes.
SHAPE II
The SHAPE II task force held its first meeting in late July to examine the new data and begin discussing the new guidelines, which will be finalized and announced during the November AHA meeting in Chicago, Naghavi said.
"The primary focus of SHAPE II will be the vulnerable patient -- people who are going to have a heart attack ... in the near future," he said.
Major changes in the SHAPE screening recommendations will reflect troves of new data generated in coronary artery calcium progression studies since 2006, as well as CIMT and 3D ultrasound carotid plaque imaging, recently validated in the High-Risk Plaque (HRP) trial.
"There will be a major update on carotid ultrasound based on the findings of the HRP trial" in some 6,000 patients who underwent CIMT assessment with 3D ultrasound, Naghavi said. Those results will also be presented at the 2010 AHA scientific sessions.
The HRP initiative BioImage study, led by Valentin Fuster, MD, PhD, from Mount Sinai School of Medicine in New York City, enrolled nearly 6,100 participants. The group was screened with ultrasound of the carotids and aorta as well as low-dose cardiac CT. Those found to be at high risk in either of these exams underwent subsequent coronary CT angiography (CTA), cardiac MRI, or PET, and the study called for patients to be followed for a minimum of three years.
The SHAPE II recommendations will also include some minor adjustments in the recommended screening ages that will "open a new window on prevention for a younger population because we do care about early prevention," Naghavi said.
Other changes in the recommendations will be the use of biomarkers such as C-reactive protein, as well as certain genetic biomarkers that have been carefully screened for appropriateness, he said.
"Framingham-based risk assessment will no longer be the entry point for screening," he said. "We're going to have a checkbox for certain markers and factors to make it easier for doctors to practice cardiac risk assessment."
The screening of at-risk adults will no longer be one size fits all, he said. SHAPE II will include special recommendations for populations in stressful or high-risk occupations such as firefighters and law enforcement personnel; research shows that these individuals can have four or five times the risk of those in less stressful jobs.
As for CT, the retesting interval recommendations (currently one to five years) for coronary artery calcium scoring will be clarified and adjusted to reflect the results of recent progression studies, which recommend different rescanning intervals based on the amount of calcium present in the baseline exam and other factors.
Making up for CAC's shortcomings
Along with coronary artery calcium, the presence of "soft" coronary artery plaque in significant numbers of asymptomatic individuals with zero calcium is also considered a potential risk. For this reason carotid ultrasound screening with 3D plaque assessment is going to be very helpful in catching those at-risk individuals whom coronary artery calcium scoring might miss. Results of the HRP initiative, to be presented at the November meeting, will show that the combined approach is very effective, Naghavi said.
"3D came to our aid in a big way," Naghavi said of the HRP results. "Carotid [US] has been given a major role" in the SHAPE II guidelines.
But SHAPE I guidelines called for screening with either CT or ultrasound. Under the new regime, will individuals need to have both scans?
That question is currently being debated by the SHAPE II task force, Naghavi said. When the final recommendations are issued, some individuals could be recommended for the second scan.
By Eric Barnes
AuntMinnie.com staff writer
August 17, 2010
Related Reading
Coronary calcium usually ignored on chest CT, August 12, 2010
Ultrasound finds high heart disease risk in some low-risk women, July 7, 2010
Coronary calcium score doesn't help predict risk in low-risk men, June 7, 2010
CT calcium scores boost value of cardiac risk factors, April 28, 2010
Texas-sized heart screening law set for September debut, August 17, 2009
Copyright © 2010 AuntMinnie.com