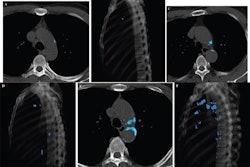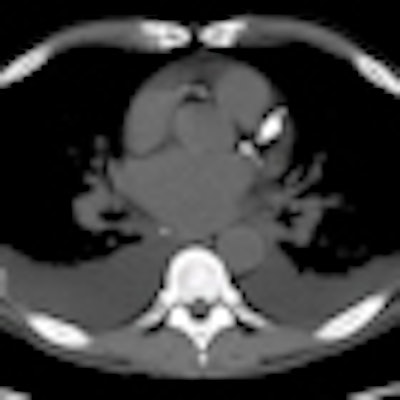
Radiologists often fail to report coronary calcium detected on chest CT scans. By ignoring it, they miss not only the chance to detect potentially serious heart disease, but an important opportunity to evaluate the chances of lowering a patient's risk of heart attack with treatment, say researchers in Detroit and Chicago.
Heart disease, the No. 1 cause of death among adults in the U.S., is strongly associated with the presence and extent of coronary artery calcium. But detecting calcium doesn't require a dedicated coronary artery calcium scan or coronary CT angiography.
Calcium can be seen in large numbers of ungated chest CT scans generated for many reasons. But radiologists are ignoring most of the calcium deposits they run into, a study presented in July at the Society of Cardiovascular Computed Tomography (SCCT) meeting in Las Vegas concluded.
Are radiologists shirking their responsibility to report these findings?
"That was the way I interpreted it until I realized there are no guidelines, so the real issue is that they're not doing the job that was never defined for them to do," said lead author and cardiologist Kim Williams, MD, in an interview with AuntMinnie.com.
"I've had several conversations with radiologists, and they all feel this is something that should be done, but they all admit they focus on the reason for the test -- the test is not cardiac, and so they may mention [coronary artery calcium] or not," said Williams, who is a professor of cardiology at Wayne State University School of Medicine in Detroit.
Coronary artery disease "leaves clues in the thousands of ungated chest CT scans" acquired every day for noncardiac purposes," he said. "The presence of coronary artery calcium is a strong predictor of risk for myocardial infarction."
The study aimed to evaluate the presence of coronary artery calcium on ungated chest CT scans acquired for other purposes, concentrating on the highest-risk coronary artery segments for stenosis.
"Our main message was letting people know when their left main proximal and anterior descending arteries had stenosis," Williams said.
To that end, the research team retrospectively evaluated 355 patients (204 women; mean age, 63 years) at the University of Chicago, who had known (n = 136) or suspected (n = 219) coronary artery disease.
SPECT myocardial perfusion imaging (MPI) was performed in 341 patients, and it was scheduled but not performed in 13. Noncardiac CT scans, including 105 without contrast, were performed within a month of SPECT for a variety of noncardiac indications.
"We cut it off at folks who had [both exams] within a one-month interval, so there couldn't be substantive changes in status" between the tests, Williams said. "We had the luxury of having lots of patients."
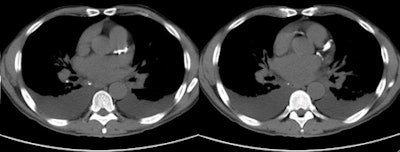 |
| Noncontrast images of the thorax in a patient presenting with dyspnea demonstrate bilateral pleural effusions and four-vessel coronary calcification (i.e., the left main, left anterior descending, circumflex, and right coronary arteries). Images courtesy of Kim Williams, MD. |
Three experienced readers working independently reviewed all of the images for cardiovascular findings. According to the results, coronary calcium was present in 202 patients (59% of the group), but coronary artery calcium was recorded as being present in the final radiology report in just 44% of patients with calcium.
As for the most dangerous arterial segments in which to have stenoses, aka "the widowmakers," calcium was visible in the left main coronary artery in 139 patients but was reported in only 0.7% of the cases, Williams said. Calcium was visible on review of the left anterior descending artery images in 188 patients, but it was reported by name in only 1.6%.
Among patients with visible calcifications that were reported at review, only six of 612 calcified arteries were actually specified by name, including:
- 1 of 138 left main arteries with calcium
- 3 of 187 left anterior descending arteries with calcium
- 1 of 137 circumflex arteries with calcium
- 1 of 150 right coronary arteries with calcium
In the SPECT MPI subgroup, presence of coronary calcium was associated with a higher summed stress score than absence (p < 0.01), the authors noted.
Williams acknowledged that ungated CT scans can distort the amount of visible calcium due to motion artifacts, but he said that reporting it isn't a problem because there is no attempt to quantify the calcium, evaluate soft plaque, or perform any other kind of assessment for which the ungated CT images would be inadequate.
Going forward, Williams said, he'd like to see the American College of Radiology (ACR) take its existing language for identifying coronary artery calcium on dedicated heart scans and apply it to chest scans acquired for noncardiac indications -- and include the requirement as part of the organization's cardiac CT training.
"The requirement would be to qualify, not necessarily quantify, the presence of coronary artery calcium in nongated CT scans," Williams said. And although Williams believes the onus should be on the medical societies to set the standards, imaging professionals shouldn't wait for a new set of rules to improve their reporting habits.
"I haven't met a radiologist yet who, when I showed them the thing in the left main, didn't say, 'This is important; I should actually say something about it,' " Williams said. "They all agree. We just need to change the practice."
By Eric Barnes
AuntMinnie.com staff writer
August 12, 2010
Related Reading
Coronary calcium score doesn't help predict risk in low-risk men, June 7, 2010
CT calcium scores boost value of cardiac risk factors, April 28, 2010
Coronary CTA best next test for positive stress patients, April 23, 2010
A normal coronary artery calcium score is reliable for several years, March 12, 2010
Does coronary calcification accurately predict occlusion? Experts disagree, February 19, 2010
Copyright © 2010 AuntMinnie.com