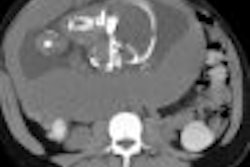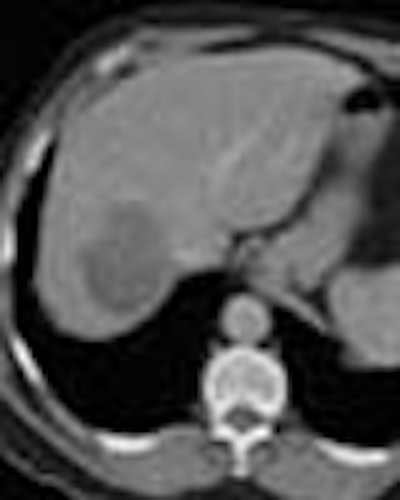
Patients who respond to chemotherapy for colorectal liver metastases should be given the same chance to undergo radiofrequency thermal (RF) ablation as nonresponders, according to a study presented at the November RSNA meeting. Given equivalent tumor status, both groups fared equally well.
"There is no significant difference in the outlook of these two groups in survival," said Dr. Alice Gillams, a radiologist at London's Middlesex Hospital. Gillams talked about her team's experience with two groups of patients of roughly equal tumor size and number. One group had disease that had been downgraded by chemotherapy, and the other group had not responded.
"The aim of our study was to see if chemo responders did as well as the rest of our patients," she said. The researchers had hypothesized that chemotherapy patients wouldn't respond as well, but they did, and only the extent of disease at the time of ablation affected the outcome, Gillam said. However, the use of chemotherapy did not increase survival rates.
"Despite many, many trials, there is as yet no significant improvement in survival with chemotherapy in correlation with metastases," she said. The situation could change with the introduction of new and better chemotherapy agents currently in clinical trials, she added.
Since 1995 the group has treated 160 patients with hepatic metastatic lesions. They performed thermal ablation on a total of 101 patients, 70 of whom had received chemotherapy, nearly all with systemic administration. Forty-eight of 70 patients received 5 FU of folinic acid. The rest received Irinottecan, Mitomycin, or Oxaliplatin, or a combination of the three.
"Of the 70 who received chemotherapy, 49 responded with a reduction in tumor size, and 36 responded but chemotherapy had to be interrupted because of toxicity," she said.
Between 1995 and 1997, thermal ablation consisted of interstitial laser photocoagulation, while subsequent ablations were performed with water-cooled, high-power radiofrequency.
"Forty of our patients were treated with laser only, 64 with radiofrequency only, and 12 started off with laser, and had radiofrequency for subsequent metastases later on in course of their disease," Gillam said. "The mean maximum diameter of our metastases was 4 cm, but there was quite a wide range (4-12 cm), and the mean number of metastases was 2 but it varied up to 20."
There were wide variations in outcomes as well, Gilliams said, showing CT images of two patients with metastatic liver disease. The first had large lesions that responded dramatically to chemotherapy. Two small remaining metastases were ablated with RF in January 1999, and the patient remained free of residual disease in May 2000.
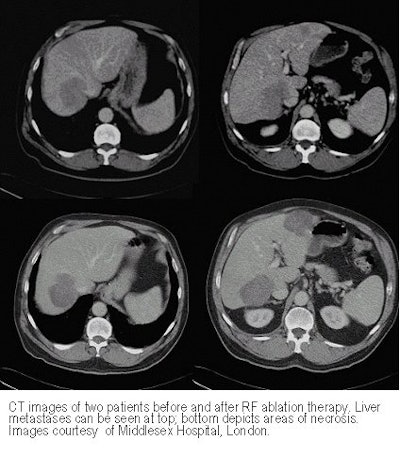
But treatment was not always successful.
"This is the other side of the coin: a patient who at first scanned in October 1997 with lots of little areas of metastases, responding initially to chemotherapy, so that in May 1998 there was very little residual disease," Gillam said. "We treated her with radiofrequency , but as the chemo response faded, she developed multiple lesions, 10 or 12 more metastases [surrounding the area of necrosis]."
Overall results were encouraging. Median survival time from diagnosis of liver metastases was 44 months for patients with 5 or fewer tumors of 5 cm or smaller, and 32 months for those with more extensive disease.
The median survival time was essentially the same for both groups of patients. What matters is the extent of disease at the time of thermal ablation, not the extent of disease prior to chemotherapy, Gillam said.
"While ablated chemotherapy responders tended to do less well, this did not reach significance, so we feel it's reasonable to offer these patients thermal ablation."
By Eric Barnes
AuntMinnie.com staff writer
January 24, 2001
Related Reading
Radiofrequency ablation treats unresectable HCC in patients with cirrhosis, October 10, 2000
Update on interventions for malignant liver tumors, February 15, 2000
Click here to post your comments about this story. Please include the headline of the article in your message.
Copyright © 2001 AuntMinnie.com