Breast imaging experts are criticizing a recent study that questioned whether common cancer screening tests such as mammography actually extend lives.
The experts have described the study and its results, published August 28 in JAMA Internal Medicine, as "invalid," "specious," and an example of "alternative facts" surrounding breast cancer screening.
"The authors failed to acknowledge that they are drawing conclusions from studies that were not designed to answer the question they have raised and lack the statistical power to support their conclusions," said Daniel Kopans, MD, from Harvard University.
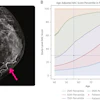
Researchers for the JAMA article sought to evaluate potential ties between several cancer screening tests and life-days gained. They gathered data from large-scale randomized clinical trials with long-term follow-up for several common cancer screening types. For imaging, this included mammography and low-dose CT for lung cancer. Of the tests, the study authors found that only sigmoidoscopy for colon cancer led to significant increases in life gained.
They also reported that mammography led to zero days gained, with a range of between -190 to 237 days, and that CT lung cancer screening led to 107 days gained on average, with a range of between -286 days to 430 days.
Design flaws?
Since then, breast imaging experts have pointed out alleged flaws in the study's design and highlighted potential consequences to patient health.
László Tabár, MD, professor emeritus of Uppsala University in Sweden, suggested that the study authors did not highlight that randomized controlled trials evaluate the impact of an invitation to screening but not the impact of screening participation. He told AuntMinnie.com that this "causes the authors to considerably underestimate the life-years preserved by participating in screening."
"It is misleading to pool these two groups under one term 'screened' and then study the 'life-years gained by screening,' " he added. "The meaningful objective would be assessing the life-years not lost to cancer in women who participated in screening, but that requires data according to detection mode on the individual level."
The study used two mammography studies from 1989 that were led by Tabár and colleagues. Tabár said that the use of all-cause mortality can give "seriously misleading results."
"Comparing 'dying from anything' among all subjects in each arm is an inappropriate study approach since the impact of participating in screening on all-cause mortality must be assessed only on subjects who actually participated in the screening examination and had a breast cancer diagnosis, and not on women who participated in screening but never had a cancer," he said. "One cannot expect that mammography screening will influence all-cause mortality in the large majority of women who do not develop breast cancer."
Tabár also remarked that a 50% reduction in breast cancer mortality among women who regularly participate in mammography screening can be thought to also reduce all-cause mortality significantly among women with breast cancer, since breast cancer-specific mortality constitutes a large part of all-cause mortality.
"It is remarkable that opponents of screening are enthusiastic about an endpoint which in more than 90% of cases is not potentially causally related to the intervention," he said.
Whacked moles
Kopans meanwhile also spoke with AuntMinnie.com on the study's claim that all-cause mortality is unaffected by cancer screening. He previously led a review of nonscientifically derived "moles" that have been "whacked" by science. Here, the failure to reduce all-cause mortality was listed as "Mole 27."
"The implication is that although they do not die from breast cancer, early detection and its consequences result in deaths from other causes so that deaths among screened women from 'all causes' is unchanged," he said. "If this is correct, then, although screening reduces deaths from breast cancer, it must, in some way, lead to an increase in deaths among screened women from some other reasons."
Kopans also pointed out that 3% of U.S. women die each year from breast cancer. If that is reduced by 30%, this will be a reduction of 1% in the total number of deaths from all causes each year.
"In order to show that a reduction of 1% in deaths is a significant reduction, we would need enormous numbers of women in a trial to prove that the clear reduction in deaths from breast cancer 'statistically significantly' reduces deaths from 'all causes,' " he said.
Kopans also cited successful efforts for breast cancer screening programs in reducing breast cancer-related deaths as suggested by previous reports.
"While we wait for a universal cure, instead of wasting time and resources devising 'alternative facts,' we should be developing better ways to detect more breast cancers at a time when cure is possible," he said.
An unfair test
Mary Newell, MD, from Emory University and President of the Society of Breast Imaging's board of directors, also said the study group's approach for assessing the value of certain screening tests is "an impractical and unfair litmus test."
"This is the hypothetical doctor-patient conversation I pictured in my head when I read this paper: 'I have good news and bad news about your screening mammogram," Newell said. "The good news is that women who undergo routine screening are up to 48% less likely to die of breast cancer. The bad news is it can't prevent your neighbor from getting hit by a bus. So, I think we should skip it."
Newell added that since each condition being screened for is relatively rare in and of itself, randomized trials would have to enroll millions of participants to prove statistically significant decreases in all-cause mortality.
"Instead, the appropriate proof of concept for a screening exam is that it results in a decrease in deaths from the condition being screened for," she said. "Screening mammography has been shown to do that in multiple randomized and observational studies."