A substantial number of women may decide not to return for recommended diagnostic breast imaging due to insurance deductibles, suggest findings published April 4 in Radiology.
Researchers led by Dr. Michael Ngo from Boston Medical Center also found that over one in five women would skip screening altogether due to deductibles, a trend they described as "concerning." Additionally, women from racial minority groups and those in a lower income bracket "disproportionately" make up women who may delay their breast imaging care due to out-of-pocket costs.
"Radiologists can use this information to advocate for legislation that would cover diagnostic imaging without any copayment or out of pocket expenses," Ngo told AuntMinnie.com.
The Affordable Care Act mandates that most private health insurance plans, Medicaid, and Medicare cover screening mammography for women ages 40 to 75 at no cost to patients. However, this does not cover follow-up diagnostic imaging for when abnormal findings are present on mammography.
Ngo and colleagues believed that the high number of people with out-of-pocket payments that come with high-deductible health plans may lead to less adherence to follow-up imaging recommendations. They wanted to explore the relationship between insurance type and patient willingness in undergoing indicated breast imaging.
The study authors collected survey data from 714 women who responded to the hypothetical statement (statement one), "If I knew that I had to pay a deductible for the additional imaging [to make sure my screening mammogram is normal], I would skip this additional imaging." They also collected data from 707 women who responded to the hypothetical statement (statement two), "If I knew that I had to pay a deductible for follow-up tests, such as imaging or biopsy, after screening mammogram, I would not undergo screening for breast cancer."
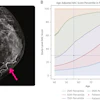
The researchers found that 21.1% of respondents (n = 151) agreed they would skip imaging, with another 19.5% (n = 139) being undecided. The groups with the highest percentage of women who would skip additional imaging were those identifying as Hispanic (30 of 91 patients, 33%), women who were high school-educated or less (48 of 155 patients, 30.9%), women with an annual household income of less than $35,000 (50 of 185 patients, 27%), and women with Medicaid or no insurance (68 of 216 patients, 31.5%).
For statement two, 18.2% (n = 129) agreed that they would skip screening mammography if they knew that they had to pay a deductible for follow-up tests, with another 16% (n = 113) being undecided. The groups most likely to skip screening mammography were women who self-reported as other race or ethnicity (19 of 72 patients, 26.4%), women who had high school education or less (42 of 155 patients, 27.1%), women with an annual household income of less than $35,000 (43 of 182 patients, 23.6%), and women with Medicaid or no insurance (60 of 214 patients, 28%).
The researchers suggested that such behaviors may lead to delays in breast cancer diagnosis and treatment. They called for legislation and policies to address financial barriers, such as eliminating out-of-pocket costs for screening and diagnostic imaging. Several states have passed bills covering diagnostic imaging without any copayment or other related expenses. These include New York, Connecticut, Illinois, Georgia, Texas, Louisiana, and Colorado.
"In addition, breast imaging practices could screen patients with high-deductible health plans for financial difficulties," Ngo said. "Those that need help can then be connected to programs that may provide them financial support."
Ngo also told AuntMinnie.com that while the team isn't planning more research in this area, a prospective study comparing the diagnostic imaging compliance rates, mortality rates, and treatment delay between women with high-deductible health plans and women without a deductible "would be a reasonable next step."