The effectiveness of breast and prostate cancer screening programs has been overstated, according to an editorial published October 21 in the Journal of the American Medical Association.
Mammography advocates have been quick to criticize the editorial, but the piece already appears to be having an effect in public policy circles: The American Cancer Society (ACS) reportedly is planning to revise its guidelines on screening for breast and prostate cancer as a result.
According to the editorial, the incidence of breast and prostate cancers has increased after the launch of screening programs and has never returned to prescreening levels, indicating that the majority of these cancers are early stage and may not pose a risk to patients. Authors of the editorial are Dr. Laura Esserman and Yiwey Shieh at the University of California, San Francisco (UCSF) and Dr. Ian Thompson at the University of Texas Health Science Center at San Antonio (JAMA, October 21, 2009, Vol. 302:15, pp. 1685-1692).
And the incidence of regional cancers hasn't decreased at a comparable rate, said Esserman, director of UCSF's Carol Franc Buck Breast Care Center and co-leader of the breast oncology program at the Helen Diller Family Comprehensive Cancer Center.
"The bottom line is that screening has limitations," Esserman told AuntMinnie.com. "People need to be aware that screening can pick up cancers that aren't necessarily dangerous."
Breast cancer and prostate cancer make up 26% of all cancers in the U.S., according to the JAMA piece. For both, women and men with the disease have much better outcomes when it is localized versus advanced (five-year survival rates for breast cancer are 98.1% for localized cancer versus 31.7% for advanced; for prostate cancer, the rates are 100% versus 31.7%, respectively).
Screening protocols are effective in finding cancer, but the increase of early cancers detected isn't necessarily beneficial, Esserman wrote.
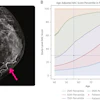
"The introduction of an optimal screening test should be followed by an increase in the rate of early disease followed by a decrease in regional disease while the overall detection rate remains constant," she wrote. "[But after 20 years of screening,] the absolute numbers of more advanced disease have not decreased nearly as much as hoped for either cancer."
Current screening protocols for breast cancer and prostate cancer find slow-growing or relatively harmless cancers but miss more aggressive cancers, according to Esserman.
"We can't count on screening to fix the [whole] breast cancer problem," she said. "We're not going to get more out of [screening programs] than we already have. Aggressive cancers show up in between screenings, and we need to invest resources to determine who's at risk for those kinds of cancers, then develop better treatments, more tailored strategies."
The editorial seems to echo, at least in part, controversial research published in the past few years by Dr. Per-Henrik Zahl, which has hypothesized that more frequent mammography screening intervals find some cancers that might otherwise "spontaneously regress" and would pose no threat were they not discovered.
"Mammography screening detects a lot of subclinical cancers that will never become clinical," Zahl told attendees of the American Society of Clinical Oncology's (ASCO) Breast Cancer Symposium, held this month in San Francisco. "But it's considered unethical not to remove [the lesion] if it has been diagnosed."
The UCSF team's verdict? What's needed are screening tests that can help clinicians distinguish between minimal-risk cancers and high-risk ones -- such as molecular tests like Redwood City, CA-based Genomic Health's Oncotype DX or Huntington Beach, CA-based Agendia's MammaPrint -- and reduce treatment for low-risk disease, as well as tools for physicians and patients that help them make informed decisions about screening, biopsy, and treatment, according to Esserman.
"The problem is not whether screening is good or bad," she said. "We're not saying people should stop screening, but we don't want people to be falsely reassured, either. The general assumption has been that if we can find cancer early we can treat it, but that's not proving to be so. Screening for these diseases should be tailored for high and low risk."
ACS weighs in
The editorial is already casting ripples. The American Cancer Society is reportedly planning to release a statement indicating that the benefits of screening may have been oversold in the past, and that screening comes with a risk of overtreatment, according to a front-page article published October 21 in the New York Times.
The article prompted the society to issue a statement by chief medical officer Dr. Otis Brawley conceding that while breast and prostate cancer screening programs have their limitations, men and women should continue to get screened for these diseases.
"While the advantages of screening for some cancers have been overstated, there are advantages, especially in the case of breast, colon, and cervical cancers," Brawley said. "Mammography [screening] is beneficial in that it saves lives, but it is not perfect. It can miss cancers that need treatment, and in some cases finds disease that does not need treatment. Understanding these limitations will help researchers develop better screening tests. The American Cancer Society stands by its recommendation that women age 40 and over should receive annual mammography, and women at high risk should talk with their doctors about when screening should begin based on their family history."
The society stands by its recommendation that men should talk to their doctors and make an informed decision about whether or not to receive prostate cancer early-detection testing, Brawley also affirmed.
For a Second Opinion on the JAMA editorial by Dr. Daniel Kopans of Massachusetts General Hospital in Boston, please click here.
By Kate Madden Yee
AuntMinnie.com staff writer
October 22, 2009
Related Reading
Shock and awe over JAMA editorial, October 22, 2009
'Spontaneous regression' debate erupts anew at ASCO symposium, October 12, 2009
Most breast cancer deaths seen in nonscreened women, October 7, 2009
Study traces steady declines in U.S. cancer deaths, August 13, 2009
Living near mammography unit may improve outcomes, August 3, 2009
Copyright © 2009 AuntMinnie.com