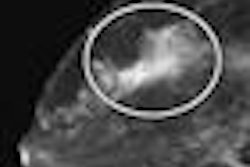
VIENNA - Sending suspicious mammograms to a third expert reader can boost the cancer detection rate of a breast screening program by a statistically significant amount, according to a presentation by German researchers at this week's European Congress of Radiology (ECR).
That was among the findings presented at a Friday afternoon session on breast cancer screening and diagnosis. Researchers presented work on a variety of topics, such as whether a change in mammography positioning techniques could reduce radiation dose, and an analysis of the factors that lead to delayed diagnosis of women recalled after suspicious screening mammograms.
In one presentation, Dr. Fritz Schaefer of the University of Kiel in Germany discussed his group's work in assessing a triple-reading program initiated as part of the QuaMaDi project, a quality management initiative in the German state of Schleswig-Holstein.
The group reviewed 102,744 mammograms from 59,514 women who were screened between 2001 and 2005. Second reads were conducted by an expert radiologist who reviewed mammography and ultrasound data.
Mammograms were sent to a third expert reader if mammography results were characterized as BI-RADS 4 or 5, and in cases of disagreement between the two initial readers in classifying lesions as BI-RADS 1/2 versus 3 versus 4/5. A total of 1,019 cancers were found in the patient population.
The study found that 24,470 cases (23.8%) were triple-read, with the third reader finding 50 additional cancers, or 5.2% extra cancers. Of these, 70% were found on ultrasound scans and 30% on mammography images.
Schaefer said that the results indicated that triple reading could have a beneficial effect on a breast screening program.
"We believe that we can improve the diagnostic standard by independent diagnostic reading," he said.
MLO versus ML
In another presentation, Dr. Jutta Peters of Brustzentrum Opernplatz in Frankfurt, Germany, reported that mammography centers might be able to reduce radiation dose by reverting back to the mediolateral (ML) view for breast imaging. The ML view was largely supplanted by the mediolateral oblique (MLO) view in the 1970s because the latter technique demonstrates more of the axillary tail of breast tissue.
There are disadvantages to the MLO view, however, Peters said. Breast anatomy can be distorted by angling the tube, and breast compression is limited by the larger amount of pectoral muscle. MLO is also more prone to pseudolesions than any other view, she said, and additional ML views are often needed, exposing the breast to more radiation.
Peters' group compared the MLO and ML views in a patient group of 38,800 women screened at their breast center from March 2007 to August 2008 using full-field digital mammography (MicroDose Mammography, Sectra, Linköping, Sweden). In total, 77,600 MLO views were obtained, and these were compared to the 520 additional ML views that were necessary for needle localization of nonpalpable lesions, preparation for vacuum biopsy, and identification of pseudolesions caused by MLO positioning.
The average radiation dose for a single MLO view was 0.646 mGy, compared to an average of 0.495 mGy for an ML view, a difference of 0.151. When both MLO views are added, the average dose climbs to 0.32 mGy.
Peters concluded by saying that while the ML view might not be the most appropriate for every woman, most women could be screened with the ML view, with an MLO projection added for those in whom the axillary tail is not visualized on ML views.
"I would suggest that we think of the ML view again as a standard view, because that's taken perpendicular to the [craniocaudal] view and that takes care of a number of problems we encounter with the MLO view," Peters said.
Delayed diagnosis
In a third presentation, Dr. Lonneke Yo of Catharina Hospital in Eindhoven, Netherlands, examined the factors that may have contributed to a delay in diagnosis for some women who were sent for follow-up after receiving suspicious mammograms.
The group studied all 290,943 screening mammograms performed on women ages 50-75 between 1995 and 2006 in a screening program in the southern Netherlands. Some 3,513 women were recalled from the group, and 1,503 women proved to have cancer. Of those with breast cancer, 6.5% of women experienced a delay in diagnosis, which the researchers defined as a diagnosis rendered more than three months after being recalled. Dutch guidelines call for 90% of women to receive a definitive diagnosis within four weeks.
In analyzing the types of cancers in the delayed-diagnosis group, the researchers found that there was a larger prevalence (26.8%) of ductal carcinoma in situ in the early-diagnosis group (15.5%, p = 0.004). In addition, there was a higher prevalence of smaller cancers, and cancers in the delayed-diagnosis group less often showed metastasis to the axillary lymph nodes (22.5% versus 48.2%). There was no statistically significant difference in tumor stage, Yo said.
Delays in diagnosis also varied considerably between the different hospitals participating in the breast screening program, Yo said. One hospital saw 5.0% of its patients experience delayed diagnosis, while another had a 9.1% rate of delay.
The biggest factor contributing to a delayed diagnosis was an incorrect BI-RADS classification, she said, such as classifying a BI-RADS 4 or 5 case as a BI-RADS 3, with 64.4% of delayed cases due to such misclassifications.
Yo said that data from the study can be used to make radiologists and breast surgeons aware of what they can do to improve quality in a breast screening program.
"It's good for them to know what is wrong and what they can do about improving it," she said.
By Brian Casey
AuntMinnie.com staff writer
March 7, 2009
Related Reading
Exceeding 'excellent': How breast centers track quality, February 17, 2009
Radiology groups need new approaches to survive in tough times, January 15, 2009
Web-based radiology dashboard aids in practice management, December 1, 2008
Home-grown databases assist radiology administrators, July 31, 2008
The best way to run your practice? Look to corporate America, April 3, 2008
Copyright © 2009 AuntMinnie.com