Radiologists overestimate their risk of being sued for mammography misses, according to a new study published in this month's American Journal of Roentgenology. Another study in the same issue found that many radiologists don't enjoy interpreting mammograms.
Fear of malpractice suits is a key influence in the declining numbers of radiologists who choose to specialize in breast imaging, recent research shows. Add this fear to the fact that many radiologists report they don't even enjoy mammography interpretation, and it's no wonder the breast imaging workforce appears to be dwindling.
But radiologists' sense of the risk of breast imaging malpractice is overrated, according to Dr. John Dick of Dartmouth Medical School in Hanover, NH, and colleagues. The group examined radiologists' reported experiences and perceptions of future lawsuit risk, as well as personal and professional factors that could be associated with fear of malpractice suits (AJR, February 2009, Vol. 192:2, pp. 327-333).
"Recruiting and maintaining radiologists in breast imaging has become problematic due in part to malpractice litigation threats and the resulting fear of litigation," the authors wrote. "Our study is the first to evaluate trends over a five-year period in malpractice lawsuit experience and perception of risk among radiologists who interpret breast imaging."
Dick's team sent questionnaires to radiologists who routinely interpret mammography exams in Washington, Colorado, and New Hampshire in both 2002 and 2006. The survey included questions on demographics, practice characteristics, and medicolegal experience and perceptions. It also included a scale that measured reactions to uncertainty in clinical situations.
The percentage of radiologists reporting malpractice claims related to mammography in the previous five years was 8% in 2002 and 10% in 2006. However, radiologists' mean estimate of the probability of being sued for malpractice in the next five years was higher by almost four times than the actual reported risk: in 2002, they guessed that they had a 41% average risk of being sued, versus a 10% actual risk found in 2006.
And the radiologists' estimates of their likelihood of being sued over the next five years varied widely: 19% estimated their risk at 10% or lower, while 25% estimated their risk at 70% or higher.
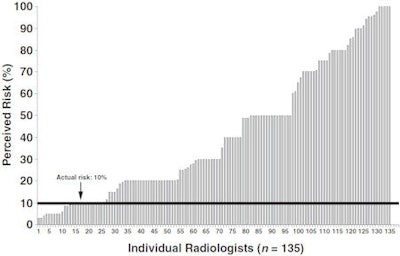 |
| Graph shows individual radiologists' estimates on 2002 survey of their own five-year malpractice risk (mean perceived risk, 41.3%; median, 30%). Actual risk noted on follow-up survey five years later in 2006 was approximately 10%. All images courtesy of the American Roentgen Ray Society. |
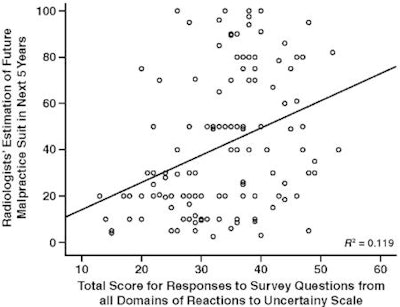
Radiologists who reported a higher perceived risk of lawsuits were more likely to have experienced a malpractice claim or to know colleagues who had. They were also more likely to have higher scores on the scale measuring anxiety caused by uncertainty in clinical situations.
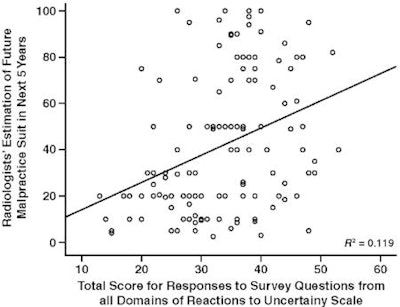 |
| Graph shows radiologists' estimate of mammography-related medical malpractice lawsuit in the next five years and total score on an instrument measuring reactions to uncertainty in clinical situations. Reaction scale can range from 10 to 60. Higher score on reaction to uncertainty scale indicates radiologist is not comfortable with ambiguity in clinical situations. Results are from 2002 survey. |
"Developing an accurate perception of malpractice lawsuit risk and understanding the characteristics of individual radiologists that are associated with an increased concern may help to lessen anxiety," Dick and colleagues wrote. "Ultimately, radiologists who can put malpractice lawsuit risks in a realistic context may be more likely to choose the field of breast imaging and maintain their interest in remaining in the field."
Not having fun yet?
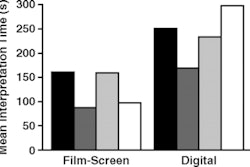
Whether or not malpractice risk for breast imaging is overrated, the finding that almost one half of radiologists who interpret mammograms do not enjoy that part of their job is yet another challenge for the modality. What's more, does their lack of enjoyment affect performance? Dr. Berta Geller at the University of Vermont in Burlington and colleagues explored the connection between enjoyment of mammography interpretation and performance and presented their work in the same issue of AJR (pp. 361-369).
The researchers included 131 radiologists from three Breast Cancer Surveillance Consortium (BCSC) registries, asking them to complete a survey about their characteristics, clinical practices, and attitudes relating to screening mammography. Results from the survey were linked with BCSC performance data for 662,084 screening and 33,977 diagnostic mammograms.
The team found that 44.3% of radiologists reported not enjoying the interpretation of screening mammograms. Those who did were more likely:
- To be women
- To spend at least 20% of their time in breast imaging
- To have a primary academic affiliation
- To read more than 2,000 mammograms per year
- To be salaried
Those who reported concern over malpractice risk, that mammography was tedious, and who had a high level of uncertainty in medical decision-making were significantly less likely to report enjoying screening mammography.
The results showed a 100% rate of satisfaction among academic radiologists, according to the researchers. Generalists were less enchanted.
"We suspect that the lower rate of satisfaction noted in our study is related to differences in the study populations; primarily, most of the radiologists in our study were generalists who included mammographic interpretation in their clinical practice and were specifically queried about this part of their practice," Geller and colleagues wrote.
The researchers found that enjoyment was not associated with screening mammography performance, although among diagnostic mammograms there was an increase in sensitivity among radiologists who said they enjoyed reading them (85.2%) compared with those who said they didn't (78.2%).
"Even though enjoyment was not significantly related to performance after adjusting for radiologists' characteristics, we can speculate how enjoyment may influence whether radiologists start and continue to interpret mammograms," the authors wrote. "Given the concern that there may not be an adequate workforce in the future to meet the increasing demands for mammography, it is important to understand why new residents are not choosing breast imaging as a specialty."
By Kate Madden Yee
AuntMinnie.com staff writer
February 9, 2009
Related Reading
Breast centers can manage malpractice risk, January 13, 2009
Treatment delays common in men with breast cancer, July 8, 2008
Walking the tightrope: The legal and regulatory impact of digital mammography, October 11, 2007
Minority women still face lag time for breast cancer diagnosis, treatment, December 27, 2006
Frivolous malpractice lawsuits uncommon: study, May 12, 2006
Copyright © 2009 AuntMinnie.com