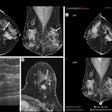
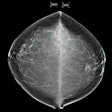
A pair of new studies in this month's edition of the American Journal of Roentgenology offers a dismal picture of the state of mammography screening: fewer women are complying with recommendations to get screened, while workforce shortages are looming as imaging professionals increasingly shun the discipline.
Although mammography is not infallible, and debate about its sensitivity and specificity continue, its use as a screening tool for breast cancer has proved to be one of the most successful public health interventions in the past 40 years. Early-stage detection of breast cancer has been linked to increased rates of mammography screening and better outcomes for women with the disease. According to the National Cancer Institute (NCI), the mortality rate for women with breast cancer decreased by 23.5% between 1990 and 2000.
But despite the effectiveness of mammography screening, a decline in use of the modality and a serious workforce shortage have come to the fore. Researchers at the Centers for Disease Control and Prevention (CDC) in Atlanta and the Center for Health Workforce Studies (CHWS) at the University at Albany School of Public Health in Rensselaer, NY, report findings from two studies that examine mammography use in the current issue of AJR (February 2009, Volume 192: 2, pp. 370-378).
The picture isn't pretty, according to Dr. Marcia Javitt, head of body MRI and genitourinary radiology at Walter Reed Army Medical Center in Washington, DC, and AJR's section editor for women's imaging.
"There are numerous definable factors that are contributing to a very disturbing decline in the use of screening mammography," Javitt said. "There's a shortage of those who read the screening mammograms; reimbursement is declining for all payments in radiology, not just mammography, and the [Deficit Reduction Act (DRA)] doesn't help; and breast imaging carries a high liability risk for reading and interpreting mammography scans. I'm not despondent, but I am worried. We've got to focus on creating policy and practice that address these issues."
Mammography use declining
Dr. Jacqueline Miller and colleagues at the CDC used data from the Behavioral Risk Factor Surveillance System for 2000, 2002, 2004, and 2006 to assess, state-by-state, the percentage of women ages 40 and older who had received a mammography exam within the past two years. The team also used data from the National Program of Cancer Registries and Surveillance, Epidemiology, and End Results Program to assess breast cancer incidence rates from 2000 to 2004.
Miller found that after a decades-long upward trend, mammography use began to decline between 2000 and 2005, rallying slightly in 2006 before once again beginning to dip. The rate fell significantly among non-Hispanic white women, ages 40 to 49.
"It's disheartening," Miller said. "Especially since, as the U.S. population continues to age, if this trend continues, we may start to see higher breast cancer incidence and mortality rates."
Estimates of mammography use rates ranged from 65.7% to 83.8% by state from 2000 to 2006 combined. In 2000, the age-adjusted percentage of women who had undergone mammography in the past two years ranged from 65.9% to 86.5%. Thirty-four states and the District of Columbia showed a decreasing trend in mammography use, ranging from -0.3% to -5.3% absolute change. Of these states, most had the largest declines between 2002 and 2004.
The study points to a relative stagnation in mammography use among women 40 and older, and understanding why some women are still not getting the recommended screening is crucial in the fight against breast cancer mortality, Miller said. Other studies have shown that women who do not have health insurance and those who have not seen their doctor within the past year are less likely to have mammography screening, which suggests that a doctor's recommendation is an important predictor of whether a woman will get a mammogram.
The attrition effect
In the second AJR study, on workforce shortages, CHWS associate director Paul Wing, Ph.D., and colleague Margaret Langelier developed forecasts of the future supply of radiologists and radiologic technologists.
Wing and Langelier used an age cohort flow model based on data they took from the American College of Radiology (ACR) on the numbers and age distribution of radiologists, as well as data provided by the American Society of Radiologic Technologists (ASRT) on RTs providing mammography services. The models predict future demand for mammography based on the age and mammography use characteristics of U.S. women in 2007.
In 2003, there were about 26,800 active radiologists in the U.S., of whom about 16,000 interpreted at least some mammograms, according to the ACR. This group of radiologists read 38 million mammograms that year. The nearly 15% of radiologists who read less than 1,000 mammograms per year read 6% of all mammograms, while the 27.4% of radiologists who read 2,000 or more mammograms per year read more than 77% of all mammograms, Wing and Langelier wrote.
Number of radiologists interpreting mammograms and number of
mammograms read in 2003 by annual volume category
|
||||||||||||||||||||||||||||||||||||||||||||
| Note: Data are from the 2003 survey of radiologists conducted by the American College of Radiology. All tables and images courtesy of the American Roentgen Ray Society. | ||||||||||||||||||||||||||||||||||||||||||||
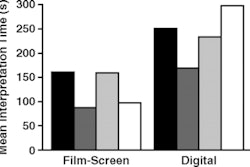
Wing and Langelier developed graph projections of the ratio of radiologists performing mammography per 100,000 women 40 years and older under three scenarios of new radiologists. They also developed the same projection for radiologic technologists providing mammography services.
 |
| Graph shows projections of ratio of radiologists performing mammography per 100,000 women 40 years old and older under three scenarios of new radiologists. Data are from Center for Health Workforce Studies, 2008, and American College of Radiology's 2003 Survey of Radiologists. |
 |
| Graph shows projections of ratio of radiologic technologists providing mammography services per 100,000 women 40 years old and older under three scenarios of new radiologic technologists. Data are from Center for Health Workforce Studies and a 2004 survey conducted by the American Society of Radiologic Technologists. |
There's a definite trend away from breast imaging specialization, according to Langelier.
"We've been noticing for a while that radiologists are much less interested in breast imaging," she said. "It may be part of the work they're required to do, but fewer and fewer are specializing in it. And those who do contribute a high percentage of their time and effort to reading mammograms."
Wing and Langelier suggested that the decline in the ratio of radiologists performing mammography, which began in 2005, will continue through 2025. And the ratio of radiologic technologists to these women will also fall.
Projected numbers of women 40 years old and older and radiologists per 100,000 population by year
|
||||||||||||||||||||||||||||||||||||||||
| Note: Data are from the U.S. Census Bureau and the 2003 survey of radiologists conducted by the American College of Radiology. Column totals may not be exact due to rounding errors. | ||||||||||||||||||||||||||||||||||||||||
Projected numbers of women 40 years old and older and radiologic technologists per 100,000 population by year
|
||||||||||||||||||||||||||||||||||||||||
| Note: Data sources are the U.S. Census Bureau and the 2004 wage and salary survey conducted by the American Society of Radiologic Technologists. Column totals may not be exact due to rounding errors. | ||||||||||||||||||||||||||||||||||||||||
Could the shortage be dealt with by simply increasing the number of studies required for radiologist certification under the Mammography Quality Standards Act (MQSA)?
The minimum MQSA requirement for radiologist certification in mammography is 960 study interpretations in a two-year period. It might seem that increasing this number would be a way to deal with the workforce shortage, but Langelier and Wing caution that this tactic needs to be handled with care: boosting the mammography volume requirement could actually push low-volume radiologists to stop reading and would compromise many women's access to the modality.
If the minimum limit of mammograms increased from 960 every two years to 1,000 every year, about 25% of current practitioners would be affected; if 75% of those read 1,000 exams per year and 25% stopped reading mammograms, there would be a total increase in mammograms read by about 719,000 per year, or 32%.
If the minimum limit of mammograms increased from 960 every two years to 2,000 every year, 54% of all practitioners would be affected; if 75% of those read 2,000 exams per year and the remaining 25% stopped reading mammograms, there would be a total increase of mammograms read by about 4.4 million per year, or 51%.
However, the effects of these increased readings would play out differently depending on location. In large cities, 21% of radiologists working in mammography interpret 5,000 or more mammograms per year, but 3.3% of radiologists in rural areas and 7.4% of those in suburban areas read this many annually. Requiring more reads per year for mammography certification could push these rural and suburban radiologists to stop reading mammograms completely.
Javitt, Miller, and colleagues, as well as Wing and Langelier, all suggest that to stop the decline of mammography use, considered and consistent effort is needed. Not only is effort needed in patient education and increased physician participation through specific recommendations to women to get a mammogram, it's also important to address impediments to professional participation in breast imaging.
"The situation isn't totally dismal," Javitt said. "But it's up to leaders in the field to craft solutions to the problems that prevent radiologists from doing mammography. We need to reward people who take on this job."
By Kate Madden Yee
AuntMinnie.com staff writer
February 3, 2009
Related Reading
Radiology subspecialization: From margins to center, August 1, 2008
Doing due diligence: What to consider in mergers with nonradiology groups, June 12, 2008
The best way to run your practice? Look to corporate America, April 3, 2008
Want to survive in a post-DRA world? Start talking, March 4, 2008
Multiple industry trends increase demand for subspecialty radiology, October 5, 2006
Copyright © 2009 AuntMinnie.com