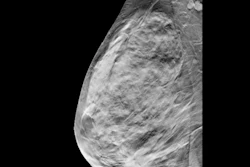
Using AI could help find more cancers on screening digital breast tomosynthesis (DBT) images, suggest findings published February 20 in the Journal of the American College of Radiology.
Interpreting DBT exams with AI assistance led to sharp increases in detecting invasive and lobular cancers, as well as those found in dense breasts. It also led to more small-sized cancers being found, wrote a team led by Kathy Schilling, MD, from Baptist Health in Boca Raton, FL.
“Use of AI was able to detect more invasive cancers without an increase in noninvasive cancers or recall rate,” the Schilling team highlighted.
Prior research has shown that DBT can increase cancer detection and decrease recall rates compared with conventional mammography. However, the researchers noted that the additional imaging volumes tied to DBT interpretation can increase reading times and lead to fatigue and burnout.
While AI has shown promise in previous research, Schilling and colleagues noted that these studies are not generalizable. The researchers highlighted a need to further evaluate AI tools in a real clinical setting.
The Schilling team evaluated breast cancer screening detection and recall rates before and after implementation of an AI detection system with DBT in an outpatient breast center. They also focused on differences in breast density and the size, stage, and histopathology of cancers detected.
Retrospective analysis included mammography audit data and screening cancers from four sites during two periods: 2018 to 2020 (pre-AI) and 2020 to 2022 (AI period). Nine dedicated breast radiologists took part in the study.
The pre-AI period included 54,440 exams (with 339 true positives) while the post-AI period had 48,742 exams (with 369 true positives). During the AI period, more cancers were detected, there were similar recall rates, more cancers were found in dense breasts, and invasive cancers were smaller on average.
Comparison of breast cancer findings before, after AI implementation | |||
Measure | Pre-AI | AI | p-value |
Cancer detection rate (per 1,000) | 6.23 | 7.57 | < 0.01 |
Recall rate | 6.97% | 6.96% | 0.47 |
Cancers found in dense breasts | 37.2% | 45% | 0.04 |
Average size of invasive cancers | 12.16 mm | 10.74 mm | < 0.05 |
Proportion of T-1 cancers | 63.1% | 70.7% | 0.03 |
Detection of ductal carcinoma in situ (DCIS) | 25.7% | 23% | 0.42 |
Invasive cancer detection rate (per 1,000) | 4.63 | 5.83 | < 0.01 |
| Lobular cancer rate (per 1,000) | 0.44 | 0.98 | < 0.001 |
With no significant change in the rate of DCIS diagnosis, this finding suggests that using AI can improve radiologists’ performance without overdiagnosing, the study authors highlighted. They also suggested that finding smaller cancers with the assistance of AI can change treatment options and outcomes for women with screen-detected cancers.
“Localized tumor burden has the potential for breast conserving surgery options without lymph node surgery and with improved radiation or endocrine therapy options,” the authors wrote.
They also called for future prospective studies and multicenter studies to evaluate AI breast cancer detection in large and diverse populations.
“Our study adds to the recent published evidence that screening outcomes are improved with the implementation of the concurrent use of AI,” they wrote.
Read the full study here.