Contrast-enhanced ultrasound (CEUS) with perfluorobutane is on par with MRI for diagnosing small-cell liver hepatocellular carcinoma (HCC), suggest findings published March 3 in Radiology.
CEUS with perfluorobutane achieved a similar performance to MRI when incorporating Kupffer-phase findings, regardless of whether patients have cirrhosis or not, wrote a team led by Yu Li, MD, from the Sun Yat-sen University Cancer Center in Guangzhou, China.
“The incorporation of Kupffer-phase hypoenhancement into [CEUS] with perfluorobutane assessment improved sensitivity for hepatocellular carcinoma [HCC] with no evidence of a decrease in specificity compared with CEUS Liver Imaging Reporting and Data System [LI-RADS] version 2017, and showed no evidence of a difference in sensitivity and specificity from MRI,” the Li team wrote.
Perfluorobutane, in addition to vascular phase, is selectively engulfed by Kupffer cells in hepatic parenchyma. This leads to sustained enhancement of liver parenchyma more than 10 minutes after contrast injection -- also known as the Kupffer phase -- where lesions that lack functioning Kupffer cells have less enhancement on imaging.
Prior studies suggest that modified CEUS LI-RADS criteria that incorporate Kupffer-phase findings increase sensitivity for diagnosing HCC without significantly affecting specificity. These results were comparable to CT/MRI LI-RADS, version 2018.
Li and colleagues compared the diagnostic performances of perfluorobutane-enhanced ultrasound and liver MRI for small HCCs in high-risk patients.
Final analysis included 365 patients with a median age of 54 who had 399 total lesions. These presented with a median diameter of 16 mm, and included 252 HCCs, 41 non-HCC malignancies, and 106 benign nodules.
The team employed two strategies: Strategy A, where lesions that were at least 10 mm with non-rim arterial-phase hyperenhancement and late and mild washout were assessed up to five minutes after injection; and Strategy B, which expanded on Strategy A by also incorporating lesions 10 mm or larger with non-rim arterial-phase hyperenhancement, no washout up to five minutes, and hypoenhancement on Kupffer-phase images.
Strategy B led to significantly higher sensitivity over Strategy A (p < 0.001), though with comparable specificity (p = 0.07). Compared with MRI, Strategy B achieved comparable results for both sensitivity (p = 0.07) and specificity (p = 0.59).
Comparison of CEUS strategies with MRI for diagnosing small-cell HCC | |||
Measure | MRI | Strategy A | Strategy B |
Sensitivity | 72.6% | 57.1% | 65.9% |
Specificity | 90.5% | 93.9% | 91.8% |
The team also studied the respective performances of both strategies in patients with and without cirrhosis. It found that both strategies showed higher specificity (p = 0.04), but no significant differences in sensitivity (p = 0.63 and 0.39, respectively) in patients without cirrhosis versus in patients with cirrhosis.
The study authors explained that the difference in specificity in cirrhosis analysis is due to distinctions in washout patterns rather than Kupffer-phase findings. This is because Kupffer-phase hypoenhancement showed no statistically significant difference between the two groups for either HCC or non-HCC nodules.
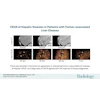
 Images in a 52-year-old man with chronic hepatitis B show a nodule categorized as LR-3 at MRI using Liver Imaging Reporting and Data System (LI-RADS) version 2018 (A-C), as LR-5 at contrast-enhanced ultrasound (CEUS) using Strategy A (D-H), and as LR-5 at CEUS using Strategy B (D-I). At contrast-enhanced MRI, (A) an axial T2-weighted image in segment VI shows a 15-mm mildly hyperintense nodule (arrow). (B) The axial arterial phase shows hyperenhancement (arrow). (C) Axial portal venous phase image shows the observation with neither washout nor enhancing capsule (arrow). (D) Conventional gray-scale US in segment VI shows a 16-mm hypoechoic nodule (arrow). (E) Image shows arterial phase hyperenhancement (arrow) at 18 seconds. (F) Portal venous phase image at 1 minute shows no washout (arrow). (G, H) Late phase at 2 minutes (G) and 5 minutes (H) shows late and mild washout (arrows). (I) Kupffer-phase hypoenhancement at 20 minutes (arrow). Pathologic diagnosis based on surgical resection was hepatocellular carcinoma. AP = arterial phase, VP = venous phase.RSNA
Images in a 52-year-old man with chronic hepatitis B show a nodule categorized as LR-3 at MRI using Liver Imaging Reporting and Data System (LI-RADS) version 2018 (A-C), as LR-5 at contrast-enhanced ultrasound (CEUS) using Strategy A (D-H), and as LR-5 at CEUS using Strategy B (D-I). At contrast-enhanced MRI, (A) an axial T2-weighted image in segment VI shows a 15-mm mildly hyperintense nodule (arrow). (B) The axial arterial phase shows hyperenhancement (arrow). (C) Axial portal venous phase image shows the observation with neither washout nor enhancing capsule (arrow). (D) Conventional gray-scale US in segment VI shows a 16-mm hypoechoic nodule (arrow). (E) Image shows arterial phase hyperenhancement (arrow) at 18 seconds. (F) Portal venous phase image at 1 minute shows no washout (arrow). (G, H) Late phase at 2 minutes (G) and 5 minutes (H) shows late and mild washout (arrows). (I) Kupffer-phase hypoenhancement at 20 minutes (arrow). Pathologic diagnosis based on surgical resection was hepatocellular carcinoma. AP = arterial phase, VP = venous phase.RSNA
“Conversely, early washout was more frequent in livers without cirrhosis for non-HCC malignancy, whereas late and mild washout was more common in livers with cirrhosis,” they wrote.
The team reiterated that these perfluorobutane-enhanced ultrasound approaches are effective and show no evidence of differences in diagnostic performance with that of MRI.
Read the full study here.