A model using ultrasonic biomarkers could help physicians identify patients with nonalcoholic fatty liver disease (NAFLD) who have advanced fibrosis, a study presented November 30 at the RSNA 2023 annual meeting found.
In his presentation, Katsutoshi Sugimoto, MD, PhD, from Tokyo Medical University in Japan discussed the performance of a model he and colleagues developed, which combines multiparametric ultrasound markers. They found that combining normalized local variance with shear-wave speed improves assessment of advanced liver fibrosis.
“The combination…improved the diagnostic performance of identifying [disease] patients compared to shear-wave speed alone, which helps physicians lead to better management and treatment decisions for patients,” Sugimoto said.
Liver fibrosis is a major prognostic factor in NAFLD, making it important to identify patients with advanced fibrosis – also known as metabolic-associated steatohepatitis (MASH). While magnetic resonance elastography shows high performance metrics in fibrosis grades of 2 and above, it has its share of drawbacks. These include its high cost, limited availability, and contraindications.
Sugimoto and colleagues sought to create an accurate model using multiparametric ultrasound to identify NAFLD patients with advanced fibrosis. It tested the model in a prospective study of 65 biopsy-proven NAFLD patients from seven sites.
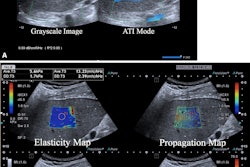
To develop the model, the team used five ultrasound markers: shear-wave speed, dispersion slope, attenuation coefficient, normalized local variance, and the echo intensity ratio of liver to kidney. These were measured using a 2D shear-wave elastography system (Aplio i800, Canon Medical Systems) immediately before biopsy. Four expert pathologists from one site scored the biopsy specimens.
The researchers found that among the ultrasound markers, shear-wave speed, normalized local variance, and dispersion slope allowed for identification of advanced fibrosis. These included area under the curve (AUC) values of 0.886, 0.805, and 0.79, respectively.
They also found that the most predictive model was the combination of shear-wave speed and normalized local variance with an AUC of 0.908. Additionally, these markers had the highest regression coefficient values in the study, including 2.34 for shear-wave speed and 6.44 for normalized local variance. These indicate a significant association with fibrosis staging.
Finally, the team reported that normalized local variance showed weak correlation with shear-wave speed, suggesting that these markers see different characteristics on liver fibrosis.
Sugimoto said that based on these results, combining shear-wave speed with normalized local variance has the highest potential for identifying NAFLD patients with advanced fibrosis. He added that the model can serve as a noninvasive and accurate tool to assess liver fibrosis.