Lung ultrasound scans helped physicians in Europe manage the treatment of two patients with COVID-19 who required mechanical ventilation. The international team behind the cases published their report on September 9 in the American Journal of Tropical Medicine and Hygiene.
The physicians used lung ultrasound scores (LUS) to determine the severity of disease in two patients before and after starting mechanical ventilation. The scores helped the team to assess how well the patients responded to treatment in order to optimize their care.
"The two presented cases suggest the need for a personalized approach in use of adjunctive therapies for refractory hypoxemia," wrote the authors, led by Dr. Charalampos Pierrakos, an intensivist at Brugmann University Hospital in Brussels. "Lung ultrasound could be an attractive bedside tool to guide their use."
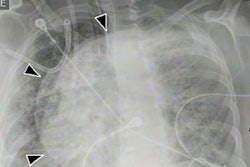
The two patients in the study were admitted to the hospital for laboratory-confirmed cases of COVID-19. The patients were in their 60s and obese, and both required invasive ventilation to manage refractory hypoxia. At admission, the CT scans of the patients showed ground-glass opacities involving 30% of the lungs.
The first patient, a 66-year-old woman, underwent invasive ventilation nine days after admission. Before starting ventilation, the authors calculated her lung ultrasound score. The LUS is the cumulative score from 12 individual sections of the lung. Each section can receive a score of 0-3, with higher scores indicating worse disease severity.
At the initial scan, the patient's cumulative LUS was 12, and none of her individual lung regions received the worst score of 3. But after the start of mechanical ventilation, the patient's total LUS shot up to 17. Several dorsal sites received a score of 3, indicating severe abnormal aeration.
Based on the score changes, the team performed an invasive recruitment maneuver by using continuous airway pressure at 60 cm H20 for 40 seconds. Following the maneuvers, the patient's LUS dropped to 14, mainly due to improvements in aeration of the dorsal areas. Her oxygen saturation also rose from 88% to 100%.
The team then moved the patient to a prone positioning. Her oxygenation and pulmonary system compliance both improved.
Similarly, the second patient, a 60-year-old man, underwent invasive ventilation 12 days after admission. An initial lung ultrasound scan showed an LUS of 11, and like the first patient, none of his lung regions had a score of 3.
For this patient, however, mechanical ventilation resulted in an improved LUS of 9. Based on the positive outcome, the team did not perform any recruitment maneuvers and left his ventilation settings the same. They also moved the patient to the prone position, and his oxygenation and pulmonary system compliance improved.
"These two cases illustrate how LUS could be useful in identifying different lung morphologies early after the start of invasive ventilation and help decide on adjunctive therapies," the authors wrote.
Lung ultrasound score has been studied by other researchers, with some findings suggesting that higher scores can indicate worse outcomes and even death from COVID-19. The new study adds to that research with further indication that ultrasound findings may also help to manage patient treatment.
Lung ultrasound also has other unique advantages for COVID-19, including that it can be used at bedside and be repeated as many times as needed. This is particularly important for assessing the immediate impacts of mechanical ventilation and potentially for performing resource management in places with limited resources.
"This has possible implications for ventilator management in resource-limited settings, with limited availability of chest computed tomography and blood gas analyzers," the authors wrote. "Tailoring invasive ventilation based on LUS findings early after the start of invasive ventilation is feasible, but this should be further evaluated in future studies."