Brain MRI findings suggest treating people with obstructive sleep apnea could reduce their risk of dementia later in life, according to a study published October 5 in JAMA Network Open.
German researchers analyzed MRI scans of patients in their early 50s and younger with obstructive sleep apnea. They found a strong link between the severity of sleep apnea and the appearance on MRI of white matter hyperintensities, a known risk factor for dementia and Alzheimer's disease.
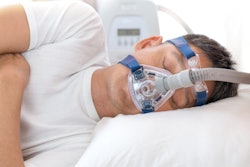
"With [obstructive sleep apnea] treatment options (e.g., positive airway pressure therapy) readily available, [white-matter hyperintensities] and associated diseases, including subsequent dementia, might be reduced," wrote first author Helena Zacharias, PhD, and a team at University Medicine Greifswald in Germany.
White-matter hyperintensities (WMH) -- areas of increased brightness on MRI scans -- are common in people older than 60 with and without cognitive impairment. They indicate reduced blood flow in small arteries deep in the brain. Exactly how they develop is unclear, but studies show they are associated with double the risk of dementia.
Chronic obstructive sleep apnea, a highly prevalent and treatable disorder, may be a contributing factor to the development of WMH, yet the studies have been small and the findings contradictory, according to the authors.
"Additional general population studies that investigate the association between [obstructive sleep apnea] and WMHs with highly standardized data collection and thorough covariate adjustment are needed," the team wrote.
In this study, Zacharias and colleagues identified 529 patients who had undergone sleep study and 1.5-tesla MRI exams during a population-based epidemiological study in Western Pomerania, Germany, between 2008 and 2012. Of those, 209 were diagnosed with mild (24%), moderate (10%), or severe (6%) obstructive sleep apnea, based on standard apnea-hypopnea index (AHI) and oxygen desaturation index (ODI) scores.
The study's primary outcome was data on white-matter hyperintensities that was automatically segmented from 1.5-tesla MRI scans. The researchers looked at total volume of hyperintensities and the numbers of WMH spots with volumes larger than 3 mm3. The median age of patients was 52.2 years.
The team found the volume of white-matter hyperintensities were significantly, positively associated with both apnea-hypopnea index (β = 0.024) and oxygen desaturation index (β = 0.033) in multivariable linear regression models adjusted for sex, age, intracranial volume, and body height. Likewise, the number of WMH spots on MRI were also significantly, positively associated with both AHI (β = 0.008) and ODI (β = 0.011).
In addition, as the severity of obstructive sleep apnea increased, ultimately so did the size and number of white-matter hyperintensities in the MRI scans, the authors found.
"Associations remained significant after thorough adjustment for additional metabolic, vascular, and lifestyle WMH risk factors, indicating a strong, independent link between OSA and WMH formation," the team wrote.
The prevalence of undiagnosed and thus untreated obstructive sleep apnea is high in the general population, the authors wrote. The associations between obstructive sleep apnea and brain hyperintensities represent a new, potentially treatable pathomechanism for WMH, they suggested.
The authors noted limitations, however, namely that no causal conclusions can be drawn from the results at this date because they are derived from cross-sectional data only.
"Future studies might investigate the effect of [obstructive sleep apnea] on WMH burden in specific [obstructive sleep apnea] populations and the effect of [obstructive sleep apnea] treatments on WMH burden in longitudinal clinical trials," the team concluded.