Brazilian researchers using diffusion-tensor MRI (DTI-MRI) found that obese teens have disrupted connectivity in regions of the brain that regulate appetite, according to a presentation delivered at the RSNA 2017 meeting.
The study findings could lead the way to better interventions in overweight adolescents and address a growing problem, wrote the team from the University of São Paulo. Obesity has more than quadrupled in adolescents over the past 30 years, according to the U.S. Centers for Disease Control and Prevention (CDC), and more than one-third of children and adolescents in the U.S. are overweight or obese.
"Childhood obesity has increased 10% to 40% in the last 10 years in most countries," lead author and doctoral candidate Pamela Bertolazzi said in a statement released by the RSNA.
DTI-MRI measures fractional anisotropy -- that is, the microscopic motion, or anisotropy, of water molecules within and surrounding the brain's white-matter fibers. Low fractional anisotropy values suggest greater disruption within the white matter.
Bertolazzi and colleagues used DTI-MRI to image the brains of 59 obese adolescents who were between the ages of 11 and 18. They compared those images with results from a control group of 61 adolescents who were a healthy weight, matching the subjects by gender, age, socioeconomic classification, and education level.
The researchers found a loss of white-matter integrity in several brain regions in the obese patients compared to the healthy controls, including the amygdala, hippocampus, thalamus, cingulate gyrus, fornix, insula, putamen, orbital gyrus, and bilateral hypothalamus. Many of these regions help regulate appetite, impulse control, emotions, and reward and pleasure in eating, according to Bertolazzi's team.
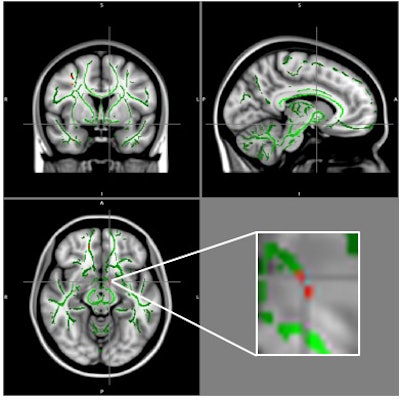
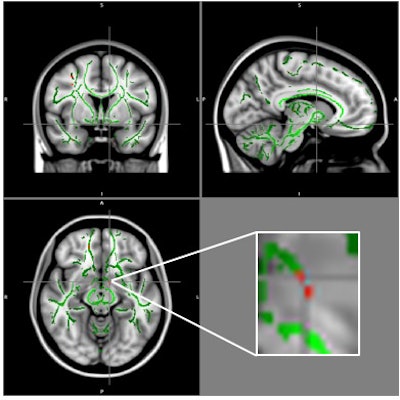 Reduction of fractional anisotropy (FA) in obese patients compared with control group (clusters in red) and FA skeleton (green), superimposed on the mean of FA images in the sample. A cluster of FA decrease is located in the left hypothalamus at the intersection of the alignment vectors. Image courtesy of RSNA.
Reduction of fractional anisotropy (FA) in obese patients compared with control group (clusters in red) and FA skeleton (green), superimposed on the mean of FA images in the sample. A cluster of FA decrease is located in the left hypothalamus at the intersection of the alignment vectors. Image courtesy of RSNA.The researchers hope the findings will offer new tools to combat the global public health crisis of obesity.
"The data reveal a pattern of involvement among brain regions that are important in the control of appetite and emotions," Bertolazzi said. "If we are able to identify the brain changes associated with obesity, this DTI technique could be used to help prevent obesity and avoid the complications associated with the condition."



![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=100&q=70&w=100)





![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)









