Diffusion-tensor MRI (DTI-MRI) shows that concussion victims have unique spatial patterns of brain abnormalities that change over time, according to a study published online June 8 in Brain Imaging and Behavior.
By detecting subtle damage to the brain by measuring the direction of diffusion of water in white matter, DTI eventually could help assess concussion patients, predicting which head injuries are likely to have long-lasting neurological consequences and evaluating treatment efficacy.
Researchers at Albert Einstein College of Medicine and Montefiore Medical Center used DTI to diagnose mild traumatic brain injury in 34 consecutive patients (19 women and 15 men; ages 19 to 64) seen at Montefiore within two weeks of injury, and again three and six months afterward. A group of 30 healthy control subjects also received DTI.
Imaging data were then analyzed using a new software tool called Enhanced Z-score Microstructural Assessment Pathology (EZ-MAP), which allows researchers for the first time to examine microstructural abnormalities across the entire brain of individual patients. EZ-MAP was developed by lead study author Dr. Michael Lipton, PhD, associate director of the Gruss Magnetic Resonance Research Center at Einstein and medical director of MRI services at Montefiore.
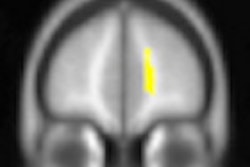
The uniformity of diffusion direction indicates whether tissue has maintained its microstructural integrity and is measured on a zero-to-one scale, known as fractional anisotropy (FA). In this study, areas of abnormally low FA were observed in concussion patients but not in the control group. Each concussion patient had a unique spatial pattern of low FA that evolved over the study period.
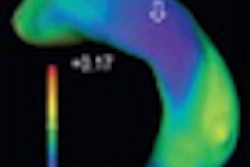
In addition, each patient also exhibited a unique, evolving pattern of abnormally high FA distinct from the areas of low FA more than one year after the injury.
The researchers speculated that high FA may be the brain's attempt to compensate for the injury by developing and enhancing other neural connections -- a new and unexpected finding.
Lipton and colleagues said that DTI with EZ-MAP analysis might provide a more objective tool for diagnosing concussion injuries and predicting which patients will have persistent and progressive symptoms.



![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=100&q=70&w=100)





![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)








