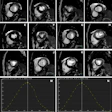
The U.S. Centers for Medicare and Medicaid Services (CMS) has initiated a review of the appropriateness of flow analysis and mapping in cardiac MR studies, which are used to evaluate cardiac valves and intracardiac shunts.
The new national coverage analysis, announced January 20 on the CMS Web site, will revisit a national coverage decision that has been in place since 1985. That decision determined that blood flow analysis and two minor cardiac MR indications were not reasonable and necessary, as follows:
The CMS has determined that blood flow measurement, imaging of cortical bone and calcifications, and procedures involving spatial resolution of bone and calcifications, are not considered reasonable and necessary indications within the meaning of section 1862(a)(1)(A) of the Social Security Act, and are therefore non-covered.
A coalition of cardiac imaging groups, including the American College of Radiology (ACR), the American College of Cardiology (ACC), the North American Society for Cardiac Imaging (NASCI), and the Society for Cardiovascular Magnetic Resonance (SCMR), had asked for the change, saying that a substantial body of evidence has accumulated since 1985 that demonstrates the utility of flow analysis.
In an interview with AuntMinnie.com, NASCI President Dr. Pamela Woodard said she welcomed the decision.
"Since 1985, extensive research has been done showing that flow is good to know," Woodward said. "We're pleased that Medicaid and Medicare have realized that, yes, there is the possibility that since 1985 there is new evidence demonstrating that flow is useful for the assessment of cardiac valves and intracardiac shunts. And we're delighted to have the opportunity to present that data."
SCMR President Dr. Charles Higgins told AuntMinnie.com the current billing codes "not allowing payments for flow studies seem, to us, to be quite ridiculous, because MRI is the best technique available for evaluating, for instance, valvular regurgitation. By not paying for it, it potentially forces the patient to have a cardiac catheterization, which is more expensive, unnecessary, and carries more risk with it."
In a December 24 letter to CMS requesting the review, the coalition noted that even the existing national coverage decision acknowledges the utility of cardiac MR angiography in its description of the modality as a noninvasive diagnostic test that "provides images of normal and diseased blood vessels as well as visualization and quantification of blood flow through these vessels" -- information that can only be obtained with flow analysis.
Blood flow quantification is one of the major techniques to diagnose valvular heart disease in adults, which is becoming more prevalent within an aging population, Higgins said. It is also "absolutely critical," he added, to determine blood flow in heart vessels of children and young adults who have been operated upon previously for congenital heart disease.
"The operation sometimes leaves the patients with significant valvular regurgitation, especially pulmonic regurgitation," Higgins said. "The only way to really measure the amount of valvular regurgitation, especially pulmonic regurgitation, is MRI. There is no other technique for this."
"We have patients that come back every year for a study because the physicians are trying to determine when to reoperate," he said. "That is based almost entirely on the amount of pulmonic regurgitation they have, as well as their ventricular function, which also is determined by MRI."
In the past, those patients were evaluated by cardiac catheterization, an invasive procedure that is more expensive than cardiac MRI. For children, cardiac catheterization "is particularly a problem because of the radiation associated with it," Higgins said.
Unusable codes
There's another big problem with the lack of coverage for flow studies, Woodward said. Prior to January 2008, blood flow analysis had its own separate current procedural terminology (CPT) codes. However, eight new CPT codes implemented last January combined blood flow analysis with other components of cardiac MRI.
But the new codes can't be reimbursed as flow remains a noncovered indication, she said. The coalition had asked for an option known as prorating, by which CMS would have simply eliminated reimbursement for the flow study.
Inasmuch as flow analysis constitutes only about 10% of the reimbursement for a typical cardiac MR exam, physicians would have simply done that portion of the study for free, Woodward said.
"We initially had requested that reimbursement for the [cardiac MR] codes containing flow be prorated," Woodward said. "However, given that CMS has indicated that this is not possible, the [national coverage analysis] gives us the option to reverse the antiquated flow national noncoverage determination."
And without the proration option, the bundled codes are useless, Woodward said.
"Because that portion is noncovered, the entire bundled code is not covered," she said. "So if you perform one of the CPT codes that includes flow, you cannot be reimbursed. It is unfortunate that one small noncovered portion of a bundled [cardiac MR] code could result in noncoverage of the entire procedure."
The bundled codes issued in January 2008 include the following:
- 75557 Cardiac magnetic resonance imaging for morphology and function without contrast material
- 75558 Cardiac magnetic resonance imaging for morphology and function without contrast material; with flow/velocity quantification
- 75559 Cardiac magnetic resonance imaging for morphology and function without contrast material; with stress imaging
- 75560 Cardiac magnetic resonance imaging for morphology and function without contrast material; with flow/velocity quantification and stress
- 75561 Cardiac magnetic resonance imaging for morphology and function without contrast material(s), followed by contrast material(s) and further sequences
- 75562 Cardiac magnetic resonance imaging for morphology and function without contrast material(s), followed by contrast material(s) and further sequences; with flow/velocity quantification
- 75563 Cardiac magnetic resonance imaging for morphology and function without contrast material(s), followed by contrast material(s) and further sequences; with stress imaging
- 75564 Cardiac magnetic resonance imaging for morphology and function without contrast material(s), followed by contrast material(s) and further sequences; with flow/velocity quantification and stress
"In general, with this starting date, it will probably take nine months to a year to get this fixed," said Pam Kassing, the ACR's senior director of economics and health policy. "We hope this would go into effect January 1, 2010. Anyone who works within the [national coverage determination] process will tell you nine months is a very fast process; 12 months is more the norm.... It depends what [CMS] does with our submission of clinical evidence."
More information on the national coverage analysis is available on the CMS Web site. As part of the analysis, CMS has initiated a 30-day public comment period on the proposed review. Between now and February 19, 2009, interested parties are invited to comment on their research or experience with flow analysis on the CMS public comment page.
By Eric Barnes and Wayne Forrest
AuntMinnie.com staff writers
January 22, 2009
Related Reading
CMS makes no change to coronary CTA payments, March 12, 2008
CMS proposes hike in cardiac PET reimbursement, October 19, 2007
Cardiac MR measures predict pulmonary hypertension, April 9, 2007
MR angiography offers greater detail in vascular imaging, March 10, 2006
4D MRI enables blood-velocity measurement in mitral valve insufficiency, June 24, 2005
Copyright © 2009 AuntMinnie.com