Can radiologists or an AI algorithm consistently identify interstitial lung abnormalities (ILA) on standard chest x-rays? Perhaps not, according to a study published April 1 in the American Journal of Roentgenology.
The finding underscores the diagnostic limitation of chest x-ray for identifying these subtle lung changes, which are increasingly recognized as early indicators of serious respiratory disease, noted a team led by Hyungjin Kim, MD, PhD, of Seoul National University Hospital in South Korea.
"[Our study found that] chest radiography was associated with suboptimal sensitivity for detection of CT-based ILA, whether interpreted by thoracic radiologists or AI," the group wrote.
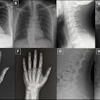
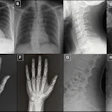
Interstitial lung abnormalities are parenchymal changes visible on chest CT -- including ground-glass opacities, reticulation, and honeycombing -- that are associated with progression to interstitial lung disease (ILD), lung cancer, pulmonary functional decline, and increased mortality. CT is the established reference standard for identifying these changes, but chest x-ray is the most widely used thoracic imaging modality worldwide due to its low cost, broad availability, and lower radiation exposure. Yet whether radiographs can meaningfully detect ILA has been unclear.
To address this knowledge gap, Kim and colleagues conducted a study that included 1,168 adults who underwent both chest CT and chest x-ray as part of health check-up programs at two Korean institutions between 2007 and 2010. Five thoracic radiologists assessed each radiograph for ILA likelihood using a five-point Likert scale; a commercially developed AI model (AIRead-CXR; Soombit.ai) evaluated the same images, then generated probability scores for indicators of ILD such as reticular or reticulonodular opacities. The group used CT findings as the reference standard.
Of the 1,168 participants, 41 had fibrotic or nonfibrotic ILA confirmed on CT imaging.
The team reported that, for detecting fibrotic ILA, radiologists achieved a mean sensitivity of 62.7% and the AI model achieved a rate of 68.2% -- a difference that was not statistically significant (p = 0.43). Both radiologists and the AI algorithm showed high specificity (97.8% and 98.7% respectively [p = 0.05]) and high accuracy (97.2% and 98.1% respectively [p = 0.04]).
But when the investigators broadened the analysis to include both fibrotic and nonfibrotic ILA, sensitivity dropped considerably, to 38.5% for radiologists and 41.5% for AI (p = 0.48) -- a result that suggests that the majority of CT-confirmed cases were missed on radiographs by both radiologists and the AI algorithm.
This finding is of concern, since the clinical significance of ILA when detected on x-ray is notable, the group explained: over a median follow-up of nearly 12 years, a positive ILA finding on x-ray was independently associated with nearly a ninefold increase (hazard ratio, 8.72; p < 0.001) in respiratory disease-related mortality after adjustment for age, sex, and smoking status, the group noted.
The study is an important reminder that a test's clinical utility depends not only on what it can confirm, but on what it can reliably rule out.
"Despite association of radiographic ILA with a clinically relevant outcome, the findings do not support radiographic screening for ILA, whether incorporating radiologist or AI interpretation," the authors concluded.
Access the full paper here.