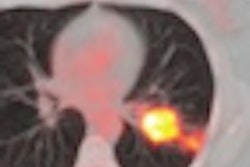
Machine learning (ML) can help clinicians predict immunotherapy response in patients with inoperable non-small cell lung cancer (NSCLC), according to a study published January 16 in Diagnostic Interventional Radiology.
The findings could help clinicians better tailor treatment for these patients, wrote a team led by Siyun Lin, MD, of Huadong Hospital at Fudan University in Shanghai, China.
"[There] is an urgent need to develop non-invasive methods to accurately predict the efficacy of immunotherapy, which could benefit a broader group of patients," it noted.
Individuals with advanced NSCLC demonstrate a range of responses to immunotherapy, and there are no reliable, accepted biomarkers to predict its efficacy, the group explained. To address the knowledge gap, Lin and colleagues conducted a study that used automatic machine learning (autoML) to predict the effectiveness of immunotherapy in 63 patients with inoperable advanced NSCLC. All patients underwent CT imaging.
The team extracted 1,219 radiomics features from areas of interest of the tumor identified on these CT exams. It then generated clinical, fusion, and radiomics models through autoML using a combination of algorithms. The group assessed the models using a multiclass receiver operating characteristic (ROC) curve.
Lin and colleagues reported the following:
| Performance of various models for predicting immunotherapy efficacy in NSCLC patients | ||
|---|---|---|
| Type of model | Training cohort | Validation cohort |
| Clinical | ||
| Accuracy | 80% | 74% |
| AUC | 0.92 | 0.88 |
| Fusion | ||
| Accuracy | 84% | 84% |
| AUC | 0.89 | 0.96 |
| Radiomics | ||
| Accuracy | 77% | 89% |
| AUC | 0.92 | 0.99 |
"The diagnostic performance of the radiomics model outperformed that of the clinical model," the group noted.
More work needs to be done to refine machine learning models and clarify their clinical relevance, according to the authors.
"[Automatic machine learning] has the ability to accurately predict the efficacy of immunotherapy and the short-term prognosis of patients with inoperable advanced NSCLC by constructing CT-based radiomics models and aiding the clinical evaluation and screening of a broader population and the development of personalized treatment strategies," they concluded.