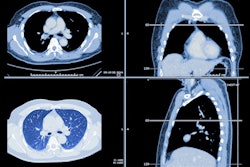
The American Lung Association's (ALA) 2022 "State of Lung Cancer" report has found that only 5.8% of Americans eligible for low-dose CT lung cancer screening have received it.
The report is the association's fifth annual, and it shows how lung cancer mortality rates vary by state: For example, two of the lowest screening rate states, California and Nevada, have rates of 1% and 1.3%, while Massachusetts has a rate of 16.3%.
Under the U.S. Preventive Services Task Force (USPSTF) most current lung cancer screening guideline, 14.2 million Americans are eligible for screening. Studies have shown that annual low-dose CT screening can reduce the death rate by up to 20%. But in the absence of early detection, lung cancer has one of the lowest five-year survival rates -- 25% -- compared with other cancers. When the disease is diagnosed early, the five-year survival rate jumps up to 61%.
The report also found the following:
- About 237,000 people will be diagnosed with lung cancer this year.
- 20.8% of lung cancer cases are treated with surgery.
- 20.6% of cases go untreated.
- People of color diagnosed with lung cancer have poorer outcomes compared with their white counterparts, with lower survival rates, and less likelihood of early diagnosis and surgical treatment.
"Increased lung cancer survival is attributable to advancements in research, better treatments, and other factors. However, lung cancer screening is the most immediate opportunity we have to save lives," ALA president and CEO Harold Wimmer said in a statement released by the association.