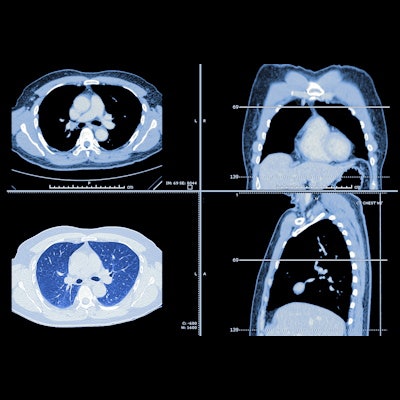
Photon-counting CT improves reader confidence when it comes to diagnosing interstitial pneumonia -- and it reduces radiation dose by more than 17%, according to research presented at the recent RSNA 2021 meeting.
The findings add to growing evidence that photon-counting CT can improve patient care, said presenter Dr. Akitoshi Inoue, PhD, of Mayo Clinic in Rochester, MN.
"Owing to the higher spatial resolution of photon-counting detector CT, prior studies have shown improved visualization of bronchi and similar appearance of lung nodules," he told session attendees.
Photon-counting-detector CT systems measure individual x-ray photons as they pass through a patient's body, in contrast to the conventional CT approach, which measures the total energy of many x-rays at one time. The first photon-counting CT scanner for commercial use was cleared by the U.S. Food and Drug Administration in September 2021.
Inoue and colleagues sought to assess photon-counting CT's impact on radiologist confidence in the diagnosis of interstitial pneumonia when compared with conventional CT technology. The team conducted a study that included 30 patients with suspected interstitial lung disease (median age, 69) all of whom underwent CT on a conventional scanner as well as a photon-counting CT system.
Three thoracic radiologists blinded to the clinical history of the study participants and scanner type evaluated images of the right and left lungs, rating the following factors on a 100-point scale (with higher values equal to likely presence of each factor):
- Ground-glass opacities (GGO)
- Honeycombing
- Lower lobe predominance
- Mosaic pattern
- Reticulations
- Traction bronchiectasis
The readers also rated the images for confidence for the probability of interstitial pneumonia (also on a 100-point scale). However, because on the confidence scale 50 represented completely equivocal findings, the absolute value of confidence scores from 50 was used for analysis (with higher scores translating to more confidence), Inoue's team noted. Finally, the readers graded image quality (overall, sharpness, presence of artifacts, and noise) on a five-point Likert scale.
Photon-counting CT improved the diagnostic confidence of the study readers for a number of imaging findings and increased overall image quality at lower radiation doses. (Conventional CT had a radiation dose of 7.88 mGy compared with 6.49 mGy for photon-counting CT, with a p-value of less than 0.001.) The team also found good intraobserver agreement (values between 0.75 and 0.9) for imaging findings such as reticulation, honeycombing, and the possibility of interstitial pneumonia.
| Photon-counting CT vs. conventional CT by clinical area | |||
| Imaging finding | Conventional CT | Photon-counting CT | p-value |
| GGO | 31.7 | 34.4 | 0.009 |
| Mosaic pattern | 35.9 | 38.6 | 0.013 |
| Peripheral lung predominance | 32.9 | 30.6 | 0.019 |
| Reticulation | 38.3 | 40.7 | 0.023 |
| Honeycombing | 42 | 42.8 | 0.054 |
| Lower lung predominance | 29.7 | 28.3 | 0.059 |
| Possibility of interstitial pneumonia | 22.2 | 24.1 | 0.059 |
| Traction bronchiectasis | 41.4 | 41.7 | 0.154 |
"Photon-counting CT increased radiologist confidence in the presence of key imaging finding indicating usual interstitial pneumonia -- for example, reticulation -- or a diagnosis other than usual interstitial pneumonia [through findings such as ground glass opacities or mosaic attenuation]," Inoue said. "And early detection of fibrosis in the lung parenchyma depicted as reticulation could contribute to timely intervention via an antifibrotic agent."
Photon-counting CT also beat conventional CT for image quality.
| Photon-counting CT vs. conventional CT for image quality | ||
| Measure | Conventional CT | Photon-counting CT |
| Sharpness | 3.82 | 4.87 |
| Overall image quality | 4.02 | 4.84 |
| Fewer artifacts | 3.91 | 3.97 |
| Less noise | 3.98 | 3.64 |
"Photon-counting detector CT provides improved image quality that translates into increased diagnostic confidence in reticulations, mosaic pattern, and ground glass opacities, which may improve imaging diagnosis of usual interstitial pneumonia," Inoue concluded.



![Axial images from unenhanced calcium score cardiac CT (left) and curved planar reformation images from CT angiography (right) show that higher long-term exposure to air pollution is associated with greater coronary artery calcium and more obstructive coronary artery disease (CAD). Top row: Images in a 68-year-old male patient with higher 10-year mean ambient air pollution exposure (7.9 μg/m3 for particulate matter measuring ≤2.5 μm in diameter [PM2.5] and 17.4 parts per billion [ppb] for NO2) with extensive CAD (coronary artery calcium score [CACS] >1,000 and obstructive CAD [≥70% diameter stenosis]). Bottom row: Images in a 57-year-old female patient with lower 10-year mean ambient air pollution exposure (6.3 μg/m3 for PM2.5 and 4.6 ppb for NO2) with no CAD (CACS = 0 and no obstructive stenosis).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/06/hanneman.r6SMLzkezo.png?auto=format%2Ccompress&fit=crop&h=100&q=70&w=100)


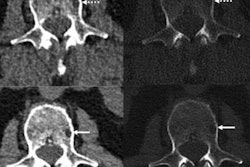
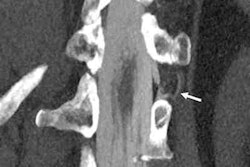

![Axial images from unenhanced calcium score cardiac CT (left) and curved planar reformation images from CT angiography (right) show that higher long-term exposure to air pollution is associated with greater coronary artery calcium and more obstructive coronary artery disease (CAD). Top row: Images in a 68-year-old male patient with higher 10-year mean ambient air pollution exposure (7.9 μg/m3 for particulate matter measuring ≤2.5 μm in diameter [PM2.5] and 17.4 parts per billion [ppb] for NO2) with extensive CAD (coronary artery calcium score [CACS] >1,000 and obstructive CAD [≥70% diameter stenosis]). Bottom row: Images in a 57-year-old female patient with lower 10-year mean ambient air pollution exposure (6.3 μg/m3 for PM2.5 and 4.6 ppb for NO2) with no CAD (CACS = 0 and no obstructive stenosis).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/06/hanneman.r6SMLzkezo.png?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)









