Monday, December 2 | 3:10 p.m.-3:20 p.m. | SSE14-02 | Room S406B
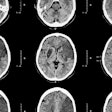
Deep-learning software for detecting intracranial hemorrhage (ICH) on CT scans can deliver faster radiology report turnaround times and reduce patient hospital stays, according to this talk.The timely reporting of critical radiology results is paramount to patient outcomes -- especially in the emergent setting, according to presenter Dr. Melissa Davis of Yale University in New Haven, CT. While they considered artificial intelligence (AI) to have broad potential for helping to optimize care, the researchers wanted to determine what effect the technology would have on timeliness metrics, especially for patients with ICH.
The researchers implemented a platform based on a convolutional neural network model on CT scanners at two imaging sites. After comparing report turnaround time and patient length of stay both before and after adopting the machine-learning platform, they found that the software produced a statistically significant decrease in report turnaround time.
"There was also a statistically significant decrease in [length of stay] for [emergency department] patients, but not for inpatients, presumably as patients with ICH were expeditiously admitted to the appropriate level of care," she told AuntMinnie.com. "Key implication being that tools like these applied to the right clinical and reading room settings could help expedite patients to the appropriate level of care and lead to improved outcomes."
Delve further into this research by taking in this talk on Monday afternoon.







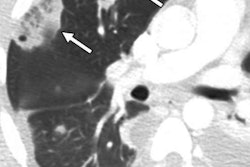
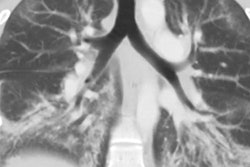








![Images show the pectoralis muscles of a healthy male individual who never smoked (age, 66 years; height, 178 cm; body mass index [BMI, calculated as weight in kilograms divided by height in meters squared], 28.4; number of cigarette pack-years, 0; forced expiratory volume in 1 second [FEV1], 97.6% predicted; FEV1: forced vital capacity [FVC] ratio, 0.71; pectoralis muscle area [PMA], 59.4 cm2; pectoralis muscle volume [PMV], 764 cm3) and a male individual with a smoking history and chronic obstructive pulmonary disorder (COPD) (age, 66 years; height, 178 cm; BMI, 27.5; number of cigarette pack-years, 43.2, FEV1, 48% predicted; FEV1:FVC, 0.56; PMA, 35 cm2; PMV, 480.8 cm3) from the Canadian Cohort Obstructive Lung Disease (i.e., CanCOLD) study. The CT image is shown in the axial plane. The PMV is automatically extracted using the developed deep learning model and overlayed onto the lungs for visual clarity.](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/03/genkin.25LqljVF0y.jpg?auto=format%2Ccompress&crop=focalpoint&fit=crop&h=112&q=70&w=112)