For acute stroke patients, researchers have used imaging scans to demonstrate that restoring an adequate volume of blood flow to brain tissue is more important in reducing damage than how quickly the flow is restored, according to a May 25 presentation at the American Society of Neuroradiology meeting (ASNR 2016) in Washington, DC.
The researchers from the University of Cincinnati examined 110 acute ischemic stroke patients who did not undergo reperfusion therapy. They found no evidence that how quickly therapy was administered affected damage to the penumbra, but they did find an association with how well collateral blood flow was restored.
In recent years, imaging has focused on evaluation of the penumbra, or the brain tissue at risk that is salvageable if blood flow is restored, as a treatment target. But few studies have examined what happens to the penumbra in the absence of reperfusion treatment to restore blood flow, said Dr. Achala Vagal, an associate professor at the University of Cincinnati, in a statement accompanying the presentation.
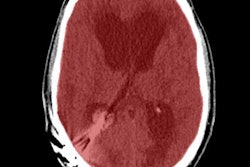
The investigators used a large, multicenter stroke registry to analyze all untreated stroke patients who had baseline CT angiography and a CT perfusion exam within 24 hours of symptom onset. The patients also had follow-up CT or MR angiography within 48 hours.
The group used the CT perfusion results to determine baseline numbers for the penumbra; follow-up CT and MRI were used to measure dead tissue.
The results showed no significant correlation between salvaged penumbra and time; however, there was a correlation between salvaged penumbra and the amount of collateral blood flow.
Future trials could help reveal the treatment implications of the results, particularly in cases of delayed or unknown stroke onset time, Vagal said. Studies with more than 110 patients will be needed to show how treatment may differ in cases with delayed treatment or unknown time of symptom onset, she added.