Tuesday, November 30 | 9:15 a.m.-9:25 a.m. | VC31-04 | Room S404CD
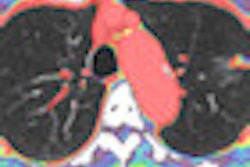
Distinguishing malignant from benign lung nodules using PET is tricky business, notably because not all lung cancers are glucose-avid. But in this Tuesday morning presentation, researchers from Kobe, Japan, will discuss how they found that perfusion CT on a 32-detector-row scanner and MRI both perform better than PET/CT for distinguishing malignant from benign nodules.Yoshiharu Ohno, MD, PhD, of Kobe University, and his group examined 43 consecutive patients with 61 nodules using three modalities: 320-detector-row perfusion CT, dynamic MRI on a 1.5-tesla scanner, and integrated FDG-PET/CT.
Nodule perfusion in CT was calculated using single-input maximum slope and the Patlak-pilot methods, along with blood volume. MRI used maximum relative enhancement ratio and maximum slope of enhancement ratio. In PET/CT, maximum standardized uptake values (SUVmax) were assessed.
All but two indices showed significant differences between malignant and benign nodules (p < 0.05) at first-pass perfusion CT. Accuracies of single-input maximum slope (88.5%) and maximum slope of enhancement ratio (86.9%) at CT were significantly higher than SUVmax in PET/CT (73.8%). CT was at least as accurate as dynamic MRI and significantly more accurate than PET/CT for detecting malignant lung nodules, the team concluded.