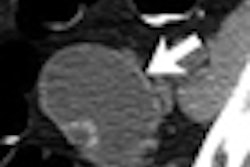
Most patients prefer virtual colonoscopy over conventional optical colonoscopy for colon cancer screening, a finding that could impact screening compliance rates if VC is more widely adopted, according to a new study published in the November issue of the American Journal of Roentgenology.
Researchers from Walter Reed Army Medical Center in Bethesda, MD, conducted a survey of 250 patients who received screening virtual colonoscopy (also known as CT colonography, CTC) at the National Naval Medical Center, also in Bethesda. They asked patients their reasons for choosing VC instead of colonoscopy, and if they received both procedures, which one they preferred.
Of the 57 patients who received both procedures, 95% preferred the virtual exam, according to a research group led by Fouad Moawad, MD. If virtual colonoscopy had not been a screening option, 91 (36%) said they would have foregone colon cancer screening.
The most common reasons for undergoing virtual colonoscopy included convenience (33.6%), recommendation by a referring provider (13.2%), and the perceived safety of the virtual technique (10.8%).
Moawad said the study indicates that offering virtual colonoscopy more widely could improve colon cancer screening rates, which remain suboptimal.
Related Reading
Study finds VC cost-effective if tiny polyps are ignored, September 9, 2010
Extracolonic findings add value to VC screening, August 24, 2010
VC not cost-effective -- unless screening rates rise, July 27, 2010
Screening VC sorts out incidental kidney lesions, June 15, 2010
5-year C-RADS analysis shows stable VC screening results, May 6, 2010
Copyright © 2010 AuntMinnie.com