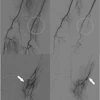
Percutaneous thermal ablation is safe and effective for treating malignant liver tumors, according to an analysis published March 24 in Radiology.
Researchers led by Gary Doppelt, MD, from St-Eloi University Hospital in Montpellier, France, found that this ablation technique is tied to a near-zero 90-day mortality and a major complication rate of about 3%.
“These results support [ablation] as a low-risk treatment with consistent safety outcomes, reinforcing its central role as a cornerstone technique within the multidisciplinary management of liver malignant neoplasms,” Doppelt and colleagues wrote.
Prior studies have shown that percutaneous thermal ablation, including radiofrequency and microwave ablation, can treat small malignant liver neoplasms. While these studies have highlighted ablation’s safety profile, the researchers noted that the exact incidence of complications varies.
Doppelt and colleagues conducted a meta-analysis to provide benchmarks for procedure-related mortality and major adverse events following percutaneous thermal ablation of small malignant liver tumors.
Final analysis included 49 studies published between 2007 and 2022. This included a total of 4,149 patients and 4,636 ablations. These studies reported adverse events after radiofrequency or microwave ablation of three or fewer liver tumors measuring 5 cm or smaller, over at least 90 days of follow-up. Imaging guidance included CT, MRI, and ultrasound, among other techniques. Two reviewers independently screened the studies, extracted data, and assessed the risk of bias.
In patients where adverse events were reported for (n = 3,149), the pooled proportion of significant adverse events was 3%. One patient died from a procedure-related incident, making for a procedure-related mortality rate of 0.01%.
Also, adverse event rates did not differ significantly between radiofrequency and microwave ablation (3.2% versus 2.6%; p = 0.41) or between hepatocellular carcinoma and metastatic tumors (2.9% versus 3.9%; p = 0.85).
The findings provide “a robust and contemporary” benchmark for procedural safety by focusing specifically on complication rates, the study authors wrote. This comes as multiple randomized trials and cohort studies have shown ablation’s efficacy.
The authors also highlighted ablation’s safety advantages for high-risk patients compared with surgical resection. Compared to ablation, postoperative complication rates in prior research are 17% for minimally invasive procedures, 19% for laparoscopic approaches, and 31% for open surgery.
“Future prospective studies with standardized adverse event definitions and data collection are warranted to clarify the impact of these variables on infection risk, procedural safety, and underreported minor complications,” the authors wrote.
The results show that “there is not one simple treatment or treatment pathway for these complex malignant neoplasms,” according to an accompanying editorial written by Michael Bettmann, MD, from Wake Forest University in Winston-Salem, NC.
Bettmann wrote that the Doppelt team’s analysis is “a useful, thoughtful, and successful attempt” to create a valid baseline for future studies in this area.
“It is encouraging that the tools and techniques for ablation, alone and as combination therapies, continue to evolve,” he added. “It is likely that the overall impressive safety of ablation only improves over time.”
Read the full study here.