Hospitals needn’t redesign their CT rooms for procedures involving anesthesia, says a lawyer who recently won a personal injury case that raised the issue.
Attorney Earl Beamon represented Cedars-Sinai Medical Center in Los Angeles during the September jury trial over a trip-and-fall case involving a staff anesthesiologist.
In 1998, Dr. Bruce Baumgarten had anesthetized a patient undergoing a CT-guided brain biopsy when, about 30 minutes into the procedure, he noticed the patient’s arm move. After ordering the technologist to stop the scan, Baumgarten rushed into the CT scan room, tripped, and then collided into the CT scanner, fracturing his hand.
Baumgarten contended that he had tripped over a blood pressure cuff cord that was approximately one foot off the ground. He proceeded to sue Cedars-Sinai for negligence in not having written policies covering the elimination of tripping hazards in the CT scan room, according to a report in Verdicts & Settlements, a supplement to the Los Angeles Daily Journal legal newspaper.
The anesthesiologist reportedly sought a $2 million settlement. A Los Angeles jury found that while Cedars-Sinai didn’t have specific written policies covering tripping hazards in the CT room, negligence didn’t cause the accident.
Had the jury held the hospital responsible for causation and awarded damages to Baumgarten, it could have set an expensive precedent for other facilities with CT-guided procedures, said attorney Beamon. "These rooms aren’t designed at the outset for anesthesia," Beamon noted. "The ultimate question was whether the CT scan room needs to be specially designed for anesthesiology, and the answer is no."
By AuntMinnie.com staff writersNovember 1, 2001
Copyright © 2001 AuntMinnie.com





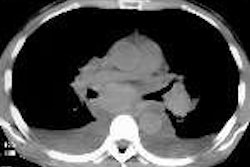










![Images show the pectoralis muscles of a healthy male individual who never smoked (age, 66 years; height, 178 cm; body mass index [BMI, calculated as weight in kilograms divided by height in meters squared], 28.4; number of cigarette pack-years, 0; forced expiratory volume in 1 second [FEV1], 97.6% predicted; FEV1: forced vital capacity [FVC] ratio, 0.71; pectoralis muscle area [PMA], 59.4 cm2; pectoralis muscle volume [PMV], 764 cm3) and a male individual with a smoking history and chronic obstructive pulmonary disorder (COPD) (age, 66 years; height, 178 cm; BMI, 27.5; number of cigarette pack-years, 43.2, FEV1, 48% predicted; FEV1:FVC, 0.56; PMA, 35 cm2; PMV, 480.8 cm3) from the Canadian Cohort Obstructive Lung Disease (i.e., CanCOLD) study. The CT image is shown in the axial plane. The PMV is automatically extracted using the developed deep learning model and overlayed onto the lungs for visual clarity.](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/03/genkin.25LqljVF0y.jpg?auto=format%2Ccompress&crop=focalpoint&fit=crop&h=112&q=70&w=112)