On October 19, a 56-year-old man arrived at the emergency department of the Inova Fairfax Hospital in Fairfax, VA, complaining of flu-like symptoms (fever, chills, chest heaviness, and a minimally productive cough of three days’ duration). He identified himself as a postal worker, and the emergency-room physicians ordered a posteroanterior (PA) projection chest x-ray and a chest CT study.
The initial evaluation in the ER revealed a widened mediastinum on the chest radiograph, and an order to rule out anthrax was sent to the radiology department. Dr. Donald Cerva Jr., the radiologist on duty, noted that the patient’s x-ray showed hilar and mediastinal masses. He also observed left-side hilar adenopathy and a small left infiltrate.
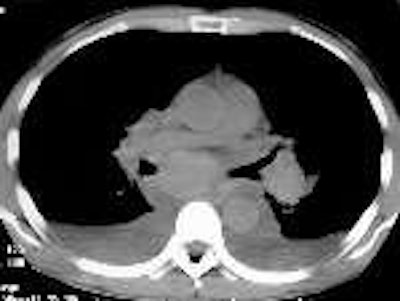
The patient was then referred for a chest CT exam. The procedure was conducted on a LightSpeed (GE Medical Systems, Waukesha, WI) spiral scanner. No contrast was used, and a standard 7-mm slice thickness chest protocol was employed.
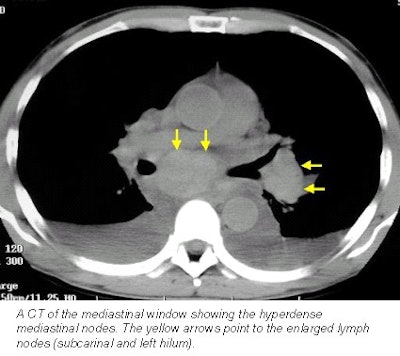
Cerva observed a profuse and slightly hyper-attenuating paratracheal, anteroposterior (AP) window, subcarinal, hilar, and azygo-esophageal recess lymphadenopathy. In addition there was diffuse mediastinal edema, bilateral pleural effusions, bibasilar airspace disease, more pronounced on the left, and thickened peribronchial tissue (seen best on lung windows).
 |
The following morning, a second postal worker, also a 56-year-old man, who worked at the same distribution center as the first patient, was admitted to Inova with a three-day history of progressively worsening headache, muscle aches, and a slight cough. Because he was linked epidemiologically to the index case of inhalation anthrax at the institution, a chest radiograph and chest CT scan were ordered.
Dr. Elise Berman was the radiologist on duty, and was aware of the earlier findings made by Cerva. She reviewed portable AP chest films and observed a widened mediastinum, bilateral hilar masses, bilateral pleural effusion, and perihilar airspace opacities.
A noncontrast CT scan was performed on the patient using the institution’s standard chest protocol. Berman found a profuse and slightly hyper-attenuating paratracheal, AP window, subcarinal, hilar, and azygo-esophageal recess lymphadenopathy similar to what Cerva had observed a few hours earlier in the first patient.
She also saw diffuse mediastinal edema, bilateral pleural effusions, and thickened peribronchial tissue. In this patient, however, bibasilar airspace disease was more pronounced on the right.
Cerva said noncontrast CT provided a good baseline for the studies.
"Contrast can always be done later if needed," she said. "Also, one patient developed some degree of renal insufficiency, which would be another reason to do a noncontrast scan," he said.
Berman offered this advice to fellow radiologists who may be called on to rule out anthrax: "If there’s any suspicion of inhalation anthrax, order a PA and lateral chest x-ray as well as a CT workup of the patient."
|
|
|
Typical radiographic findings of inhalation anthrax |
|
|
|
Chest x-ray |
|
|
|
|
|
|
Noncontrast routine spiral CT |
|
|
|
|
|
|
Information courtesy of Drs. Donald Cerva, Elise Berman, James Earls, and Mark Frank |
|
|
Dr. James Earls, the staff radiologist coordinating the radiology department’s response, said that chest imaging offered a quick and easy method of screening for advanced disease.
"The noncontrast CT has the clear advantage of being a rapidly and widely available test, which can then be confirmed with appropriate blood cultures and other tests which can take from between 24 to 72 hours."
Earls and his fellow radiologists believe the presence of enlarged hyperdense nodes depicted on the noncontrast CT, in the clinical setting of exposure to an anthrax "hot spot," along with concurrent flu-like symptoms, should be considered a positive screen for active inhalation anthrax.
Requests to rule out anthrax have picked up at the facility in the 10 days since the first cases were presented.
"We have screened well over 200 people in the ER for possible disease, and, from a radiological perspective, use the following algorithm: If a routine chest x-ray has positive findings of mediastinal widening, peripheral infiltrates, and/or pleural effusions, a noncontrast spiral CT is performed," Earls said.
The group has performed more than 30 such CT exams after positive routine chest x-rays, but none of these patients has had enlarged nodes or mediastinal edema, and subsequently none has turned culture-positive for inhalation anthrax.
"In our small sample this makes CT 100% sensitive and specific for detection of the advanced form of the disease," Earls said. "This high degree of accuracy will likely change as more cases present, but at this point I think we can agree that CT is the best imaging tool currently available, and our clinical physicians have rapidly adopted its use in the current crisis."
By Jonathan S. BatchelorAuntMinnie.com staff writer
October 30, 2001
The cases can be viewed at the Armed Forces Institute of Pathology Web site, courtesy of Dr. Jeffrey Galvin, chief of chest and mediastinal imaging. The first case is located here. The second case is located here.
AuntMinnie would like to thank Dr. Mark Frank for his assistance with this article.
Related Reading
Anthrax NPR Report, October 29, 2001
Inhalation Anthrax (B anthracis): Radiological Presentation, October 25, 2001
Anthrax Review Article, New England Journal of Medicine, September 9, 1999
Copyright © 2001 AuntMinnie.com