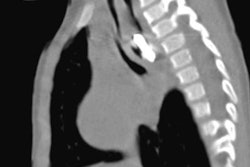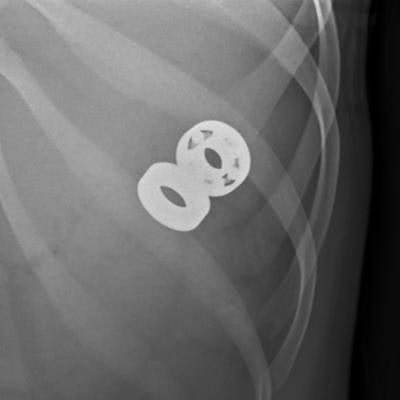
X-rays helped surgeons confirm the presence of an ingested fidget spinner toy in a patient and remove the metal parts via endoscopy, but they could not visualize plastic portions of it, according to a report published online February 22 in JAMA Otolaryngology -- Head and Neck Surgery.
The findings suggest that clinical cases like this one may be more complicated than they seem, lead author Dr. Jeffrey Otjen from Seattle Children's Hospital told AuntMinnie.com via email.
"Even if you see an object on x-ray, you can't necessarily assume you're seeing the whole thing," he said. "Complex objects like fidget spinners have parts that show up on radiography and parts that don't, and in this case, the jagged plastic part that did not show is what caused complications."
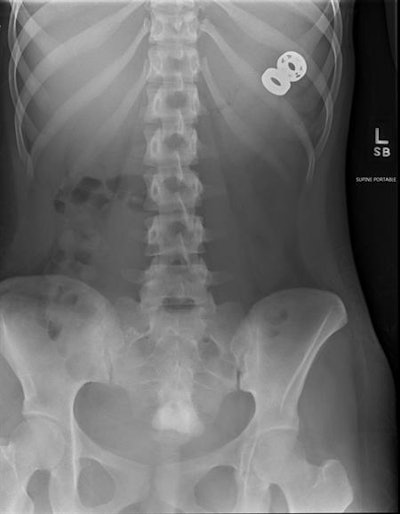 Abdomen radiograph shows the two pieces of spinner that were not surgically removed but which passed normally. Images courtesy of Dr. Jeffrey Otjen.
Abdomen radiograph shows the two pieces of spinner that were not surgically removed but which passed normally. Images courtesy of Dr. Jeffrey Otjen.A woman in her late teens with a "complex mental health history including depression and eating disorder" swallowed parts of a fidget spinner broken into three pieces, Otjen and colleagues wrote. X-ray and endoscopic evaluation confirmed the presence of parts of the object in the esophagus; they were taken out via rigid endoscopy.
Removing the toy proved challenging due to the fact that parts of it were impinging the esophagus and needed to be rotated. Follow-up x-ray three days later showed retropharyngeal gas, which prompted an additional week of intravenous feeding for the patient. Other parts of the toy passed normally some days later.
"Because the object was four times larger than the normal esophageal lumen with jagged edges and showed no movement with nonsurgical treatment, injury was likely prior to removal," the researchers wrote.
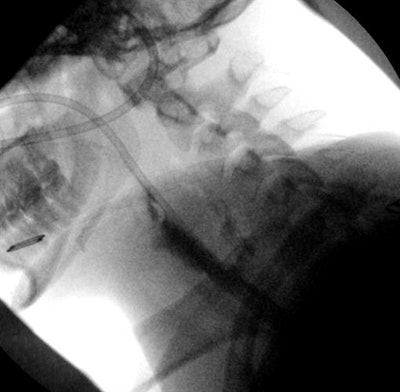 Esophagram shows a leak of contrast into the retropharyngeal soft tissues.
Esophagram shows a leak of contrast into the retropharyngeal soft tissues.In cases of foreign body ingestion, it's important to consider that there may be parts x-ray can't identify, the researchers concluded.
"Always consider that in the setting of one foreign body ingestion there could be several others that have gone unreported [or unvisualized]," they wrote.