BERLIN - Percutaneous radiofrequency ablation (RFA) and other minimally invasive interventions have become increasingly popular, thanks to their low cost and fast recovery times relative to open surgery.
Guided by real-time laparoscopic ultrasound (LUS) -- and usually static CT or MR images nearby -- physicians are treating a wide variety of abdominal tumors such as lung and kidney cancers, and even bone metastases.
But the interventionalists who perform them often end up working in the dark. The volumetric CT or MR image they've placed across the room bears little resemblance to the LUS images used to guide the RFA needle. Even worse, RFA can deform the abdomen significantly during the procedure, rendering external landmarks all but useless for guidance.
What the world needs now, according to a presentation at the 2005 Computer Assisted Radiology and Surgery (CARS) meeting, is electromagnetic tracking of the laparoscope and coregistration of the LUS with preacquired volumetric CT or MRI.
The problem
Radiologists are used to looking at CT and MR images in certain standard perspectives, such as multiplanar reconstructions, said Dr. Bradford Wood in a presentation on Saturday. However, he said, LUS images are displayed in random planes, making them impossible to compare with the preoperative CT or MRI images.
The discordant images "often lead to difficulties in usage, and there's a wide variety of skill levels and comfort levels in interpretation," he said. "You have all these layers of complexity, there's no good training method, and you end up with a difficult technology that makes it hard to translate new procedures to the community setting."
The need for laparoscopic tracking, in RFA and other procedures, led to the initiation of a collaborative study supported by academic and corporate researchers from the National Institutes of Health in Bethesda, MD; Johns Hopkins University in Baltimore, MD; Georgetown Medical School in Washington, DC; and Philips Research in Briarcliff Manor, NY, and Hamburg, Germany.
Wood, who is senior clinical investigator at the National Institutes of Health Clinical Center in Maryland, built and tested a prototype tracking system along with his co-investigators Neal Glossop of Traxtal, Jochen Kruecker and Joern Bogert of Philips Research.
There is an urgent need for better tracking during RFA and other minimally invasive procedures, Wood said, noting the problems inherent in RFA ablation of hereditary kidney tumors as an example."They're very difficult to see," he said. "You know where they are beforehand, you get to the operating room, hang the films across the room, go back to the patient, and it's very difficult to find these small lesions. Ultrasound is never physically referenced to the CT scan in the current standard of care.... You try to guess what you're looking at, and this is compounded by the fact that once you place the needle and start cooking, you're left with a gas-out effect, where the (CO2) from the ultrasound completely shadows what you see, and you're left with no information at all from the ultrasound."
Considering that the accuracy of RFA needle placement is directly related to patient outcomes in this procedure, a better solution is needed urgently, he said.
"The conventional surgeon registers, tracks, and builds a 3D model in his head, all simultaneously, based on films he has hung across the room," Wood said. "I would argue that this really should be (considered), in the future, malpractice."
The device
To solve the problem the team built an experimental workstation with electromagnetically tracked surgical tools to register real-time LUS images with preacquired CT data. Then the registration and image fusion were used to guide a tracked needle to target locations in an abdominal phantom.
The team equipped a custom-fitted electromagnetic sensor (Traxtal, Bellaire, TX) with a 9-MHz linear array laparoscopic ultrasound transducer (Philips Medical Systems, Andover, MA). The sensor sleeve, offering six degrees of freedom, was tracked by an Aurora magnetic tracking system (Northern Digital, Waterloo, CA). The tracking system was calibrated to relate the tracking system to physical and image coordinates, enabling the tip of the RFA needle to be used as a pointing device, the group wrote in an accompanying abstract.
 |
 |
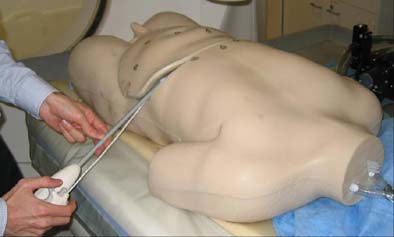 |
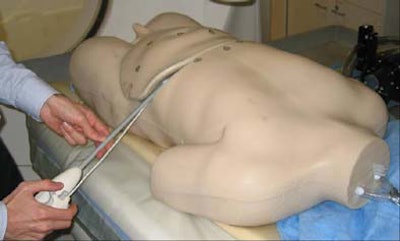
| Top, middle images: Tracked laparoscopic ultrasound prototype by Traxtel (patent pending). Bottom: Breathing phantom for testing new equipment (made by Dan Stoianovici, Johns Hopkins University). All images courtesy of Dr. Bradford Wood, who notes that the U.S. government does not endorse or warrant the usefulness of any apparatus or product used in the study, and further that the collaborating companies and investigators have filed multiple patent applications covering the devices and methods described. |
CT scans were acquired on a Philips MX 8000 scanner using a slice thickness of 2 mm with 50% overlap, and a 400-mm field-of-view, Wood said. One CT scan was used to register ultrasound image and tracking space, and following each needle placement, a second CT image was acquired to verify the needle position. Custom software was developed to calibrate and register the CT images, and provide navigational feedback for advancing the probe into an abdominal phantom.
The test
Both a static foam phantom and a breathing abdominal phantom were used in the study, Wood said.
There were 15 registrations inside the stationary phantom, and each registration had a needle placement to perform, he said. Identifying the corresponding physical positions took an experienced operator about one minute using the commercial pointer, and two minutes using laparoscopic ultrasound, the authors wrote in their abstract.
"We stuck a gel liver with targets in it ... into the (breathing) phantom, and had the targets move and tried to hit those targets using the tracking system," Wood said.
Experienced operators took about two minutes to identify the anatomic landmarks and fiducial markers that had been placed inside them. The results showed no statistically significant difference between the mean registration errors. The registration results were then used to overlay the laparoscopic ultrasound image onto the existing CT image and guide a tracked needle to a point target inside the phantom.
The displayed accuracy values of the tracked pointer, the tracked laparoscopic tip, and the LUS imaging of landmarks were 1.98 mm ± 1.00 mm, 1.36 mm ± 0.50 mm, and 1.32 mm ± 0.68, respectively, while the confirmed accuracy values (tested with subsequent CT scans) were 1.82 mm ±1.59 mm, 1.27 mm ± 0.65, and 1.88 mm ± 0.81, respectively. Preliminary results with the breathing phantom averaged between 2-3 mm, Wood said.
"The GUI (graphic user interface) view ... shows you a blending between the CT and ultrasound of your targets, and you can go back and forth between the two," he said. So when CO2 gas obscures the ultrasound view during ablation, "you can blend back and use your preoperative imaging when you most need it," Wood said.
The test produced adequate registration accuracy in a static phantom in the tracked pointer, the tracked laparoscopic tip, and the LUS imaging of landmarks, Wood concluded. The method is feasible, and can accommodate CT, MRI, or fused PET-CT for guidance when the real-time LUS is inadequate. And the system will soon be added to an ongoing trial of tracked biopsies and ablation procedures for further testing, he said.
"We all struggle to remain clinically relevant with many of these technologies, and I would argue that this is very clinically relevant, and solves a clinical problem," Wood said.
By Eric Barnes
AuntMinnie.com staff writer
June 27, 2005
Related Reading
Radiofrequency ablation effective for small renal tumors, June 24, 2005
RFA demonstrates 'surprising' efficacy for treatment of lung malignancies, April 4, 2005
RF ablation curbs colorectal cancer liver metastasis, March 30, 2005
RF ablation gains ground as lung cancer option, January 14, 2005
Copyright © 2005 AuntMinnie.com