Advanced MRI techniques can detect differences between responders and non-responders to asthma therapy as early as six weeks into treatment, according to a study presented May 11 at ISMRM in Cape Town.
The finding is from a prospective study in patients with severe asthma treated with mepolizumab who underwent phase-resolved functional lung MRI (PREFUL) and fluorine-19 (F-19) MRI to track regional ventilation changes across the lung, noted presenter Julienne Scheller, a PhD student at the German Center for Lung Research in Munich.
“Biologic treatment of severe eosinophilic asthma is successful in only 80% of patients and predictive factors for treatment response are not yet available,” Scheller said.
Up to 10% of 300 million people worldwide have severe, uncontrolled asthma. Mepolizumab is an established humanized monoclonal antibody treatment, but determining whether it is working typically requires waiting four to 12 months based on clinical symptoms and self-assessment, Scheller explained. The delay can mean prolonged treatment in patients who aren't benefiting, or premature discontinuation in those who are, she noted.
To assess whether MRI can fill the gap, Scheller and colleagues scanned 33 patients at baseline, six weeks, and three months using PREFUL, which maps ventilation across the lung region by region during normal breathing. A subset of 24 patients also underwent F-19 MRI at baseline and three months. This technique directly images an inhaled fluorinated gas as it fills the airways. Standard spirometry was also performed at the same timepoints.
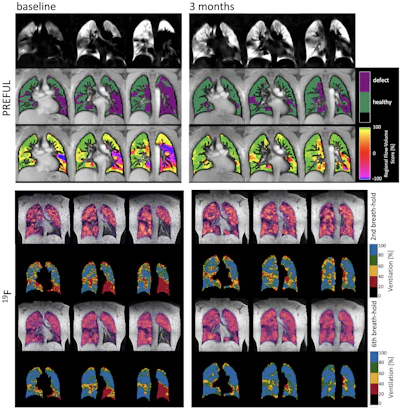 Representative PREFUL and F-19 MRI results at baseline and three months of a male responder (age: 47). First row: PREFUL ventilation images; Second row: Ventilation defect percentage (VDP) maps; Third row: Flow-volume loop (FVL) maps. VDP changed from 54% to 23% and the FVL score over the whole lung increased from 88% to 98%. Fourth and fifth rows: second breath-hold F-19 ventilation with corresponding VDP map; sixth and seventh rows: sixth breath-hold F-19 ventilation with corresponding VDP map. Second VDP decreased from 26% to 10% and 6th VDP from 16% to 3%.Julienne Scheller and ISMRM
Representative PREFUL and F-19 MRI results at baseline and three months of a male responder (age: 47). First row: PREFUL ventilation images; Second row: Ventilation defect percentage (VDP) maps; Third row: Flow-volume loop (FVL) maps. VDP changed from 54% to 23% and the FVL score over the whole lung increased from 88% to 98%. Fourth and fifth rows: second breath-hold F-19 ventilation with corresponding VDP map; sixth and seventh rows: sixth breath-hold F-19 ventilation with corresponding VDP map. Second VDP decreased from 26% to 10% and 6th VDP from 16% to 3%.Julienne Scheller and ISMRM
The F-19 scans confirmed overall ventilation improvements at three months, and one F-19 metric, time-to-fill (a measure of how many breaths it takes to adequately fill the lungs), also separated responders from non-responders, according to the analysis.
Lastly, standard spirometry showed overall improvements in FEV1 (forced expiratory volume in one second) across the group, but was unable to distinguish responders from non-responders at any timepoint.
"MRI has the advantage to capture regional differences and was sensitive enough to observe a higher treatment effect in responders than non-responders," Sheller said.
The study was single-center with a small patient population, and the group noted that larger multicenter studies are needed to validate the findings and move the techniques toward clinical use.
"Future studies should aim to validate these results in larger, multicenter cohorts," Sheller concluded.
Check out AuntMinnie's full coverage of ISMRM 2026 on our ShowCast.