Dear AuntMinnie Member,
The eroding power of private-practice radiology groups in the U.S. healthcare paradigm has many groups wondering if their hospital contracts will be next on the chopping block. But taking a few precautions can help radiology groups maintain these vital relationships.
That's according to a new article we're featuring in our Imaging Leaders Community. Associate Editor Kate Madden Yee spoke with Dr. Syed Zaidi, president of Radiology Associates of Canton, who explained his thoughts on the evolving nature of the hospital-group relationship.
Once believed to be indispensible, radiology groups are now frequently seen as replaceable by their hospital partners. To counteract this development, radiology groups must work even harder, creating good lines of communication with hospital administrators and enlisting other physicians as allies. Find out what else you can do by clicking here.
While you're in the community, check out a new article on whether more code bundling could be in store for U.S. radiology in 2016. The U.S. Centers for Medicare and Medicaid Services yesterday released its proposed 2016 rule for its Hospital Outpatient Prospective Payment System, and the proposal indicates that the agency plans to consolidate a number of its ambulatory payment classifications.
Looking for an English translation? Radiology sites next year could be paid just once -- and at a lower rate -- for procedures they used to be able to bill for twice, resulting in lower revenues. Learn more by clicking here, or visit the community at leaders.auntminnie.com.
Lung x-rays and MERS
Middle East respiratory syndrome (MERS) has become a feared disease, not only in the Middle East but also at other locations around the globe where outbreaks have occurred, such as in South Korea. Fortunately, a multicenter group has published guidelines for using conventional radiography to predict which MERS patients are at risk of dying -- and thus who should be treated more aggressively.
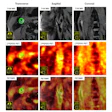
Researchers analyzed radiographs of 55 patients with MERS at a hospital in Saudi Arabia and applied a scoring system to rate the progression of pathology on the x-rays over time. They then correlated these scores with patient outcomes.
They found that radiographic score was one of the best predictors of patient mortality, and when used with clinical factors such as comorbidities, it could give healthcare personnel a good idea of a patient's prognosis. Find out how it works by clicking here, or visit our Middle East Community at me.auntminnie.com.