Dear Digital X-Ray Insider,
Computer-aided detection (CAD) is a promising technology for chest radiography studies, but when CAD algorithms are required to process data from different kinds of x-ray systems, results can vary.
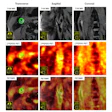
Researchers from the Netherlands believe they may have found a solution for standardizing CAD results. A group from Radboud University Medical Center in Nijmegen developed an image processing algorithm that basically "normalizes" the signal from various radiography units to something that's easier for a CAD program to analyze consistently.
The technique can make CAD more consistent when analyzing chest radiography studies for signs of tuberculosis, according to the researchers. Learn more in this issue's Insider Exclusive by AuntMinnie.com International Editor Eric Barnes.
In other news, learn how a team from Brazil used WhatsApp Messenger, a popular instant messaging app, as a diagnostic tool for radiographs.
Also, the U.S. Environmental Protection Agency this month issued final guidelines on radiation protection for federal facilities that use diagnostic and interventional x-ray. Learn more by clicking here.
Perhaps no surprise here, but researchers from Hong Kong discovered that they were able to get portable x-ray images into their PACS network faster using a wireless digital radiography system rather than a mobile unit outfitted with computed radiography plates. Find out how much faster by clicking here.
Finally, read about how chest CT referrals from abnormal x-ray studies have clinically relevant findings, and learn about Bleeper Sv, a radiation dose monitor that notifies healthcare personnel in real-time about how much dose they are receiving during cardiac catheterization procedures.
All this and more is available in your Digital X-Ray Community, at xray.auntminnie.com.