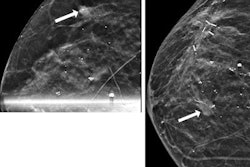
Screen-detected breast cancer in Black women is less likely to appear as architectural distortion and more likely to present with calcifications compared with white women, a team from Washington University in St. Louis has reported.
A group led by Dr. Jieqi Wang also found that Black women are more likely to have screen-detected oval or round malignant masses with nonspiculated margins on mammography, as well as circumscribed margins on sonography. The team's results were published November 17 in Clinical Imaging.
Advances in breast cancer screening have improved mortality rates in women, but racial disparities persist, the investigators noted. Previous research suggests that while the incidence of breast cancer in Black women is comparable to that of white women, mortality rates are about 40% higher in Black women.
Multiple factors may contribute to this trend, including more limited access to or underuse of screening, increased odds of later-stage diagnosis, and healthcare facility factors. But data regarding differences in imaging characteristics between the two groups are scarce.
Wang and colleagues sought to assess any breast imaging finding differences between Black and white women, accounting for molecular subtypes and histology. They looked at data from 270 Black women with 278 cancers (166 screen-detected, 112 clinically identified) and 586 white women with 599 cancers (397 screen-detected, 202 clinically identified).
The investigators found that Black women had higher rates of non-dense breast composition compared with their white counterparts (p < 0.001). This includes having almost entirely fatty composition (12% vs. 4.6%) and having scattered fibroglandular tissue (50.9% vs. 45.2%).
Also, Black women were less likely to have screen-detected architectural distortion (odds ratio, 0.38; reference is 1) and were less likely than white women to have screen-detected irregular than oval or round masses, which the researchers suggested could be due to lower use of tomosynthesis screening and screening utilization in general among Black women. They also reported that Black women are more likely to present clinically with high-density masses (odds ratio, 3.03) and showing posterior enhancement (odds ratio, 3.02).
Finally, the researchers found significant differences in tumor histology in the screen-detected cohort, including higher rates of ductal carcinoma in situ (DCIS) in Black women (42.2%) compared to white women (29%). They suggested that this trend may reflect racial differences in the use of screening mammography since this wasn't seen among the women whose breast cancer was identified clinically.
The study findings highlight that it's important to take a woman's race into consideration when it comes to breast cancer screening, according to the authors.
"Familiarity with these imaging appearances and consideration of underlying socioeconomic differences may provide breast imagers with a better framework to approach breast cancer diagnosis in the [Black] population in their clinical practice," they concluded.