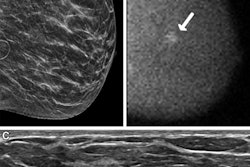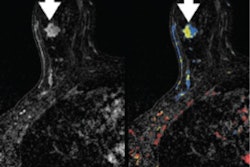
Postprocessing software shows promise for reducing the radiation dose of molecular breast imaging (MBI) -- making way for more widespread adoption of the modality for breast cancer screening in women at higher risk or with dense breast tissue, according to a study published online October 9 in the American Journal of Roentgenology.
The results suggest that "application of the image-processing software would allow performance of MBI at reduced administered activity with no loss in lesion conspicuity," wrote a team led by Dr. Ashley Tao, PhD, at the Mayo Clinic in Rochester, MN.
MBI finds more cancers, particularly in women with dense breasts, than either digital mammography (an additional 7.7 to 8.8 cancers per 1,000 women screened) or digital breast tomosynthesis (an additional 9.3 cancers per 1,000 women screened). But it imparts a radiation dose of 5 mSv to 8 mSv, which is considered too high for routine breast cancer screening, the team noted.
"Concerns have been raised because the effective dose of MBI is higher than that from two-view full-field digital mammography [FFDM] ... and from FFDM combined with tomosynthesis," the group wrote.
Tao and colleagues investigated whether using a postprocessing algorithm could cut in half the radiopharmaceutical dose of technetium-99m sestamibi for MBI exams from 300 MBq to 150 MBq. The study included data from 50 patients who underwent standard-dose MBI exams; the researchers simulated half-dose exams by summing the first half of the MBI image data.
Two radiologists interpreted the standard-dose and simulated half-dose exams using the postprocessing algorithm in either a "default mode" (the software reduced noise in the image using a mathematically calculated factor) or a "preferred filtered" mode (the software segmented the breast tissue on the image, measured the counts per pixel, and adjusted the algorithm setting based on count density).
The researchers found that the simulated half-dose images weren't conspicuous enough for the radiologist readers: The readers rated the simulated half-dose images as poorer in 92 of 100 interpretations, equivalent in six, and better in two, compared with the standard-dose images. However, the half-dose images processed with the algorithm were better visualized.
| Lesion conspicuity: Standard-dose MBI compared with half-dose, with and without algorithm | |||
| Lesion conspicuity (out of 100 readings) | Simulated half-dose images | Default filtered half-dose images (algorithm) | Preferred filtered half-dose images (algorithm) |
| Poorer | 92 | 14 | 11 |
| Equivalent | 6 | 73 | 34 |
| Better | 2 | 13 | 55 |
Reducing the dose of an MBI exam is valuable because it can lower both the radiation exposure risk and also the anxiety radiation exposure can cause patients, according to Tao's group.
"Reduction in the MBI radiation dose is of value, not because low-dose radiation causes cancer but because people fear it will cause cancer, and that fear translates into missed appointments or refusal to undergo recommended screening," the team concluded. "Implementation of the image-processing algorithm applied in this study should result in an improved acceptance of MBI and remove an obstacle to the adoption of this technology."