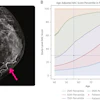
Another new analysis is questioning whether overdiagnosis is really that important to women undergoing breast screening. Authors of a study in the October issue of Medical Care believe the findings indicate that more communication is needed to convince women that they should take mammography's "harms" more seriously.
Fewer than 20% of respondents to a survey of more than 400 U.S. women knew about breast cancer overdiagnosis and overtreatment, according to the research group from the University of Minnesota. And those who do know about these mammography "harms" don't find information about them "believable or persuasive."
The researchers suggest that their findings underscore the need to better communicate mammography risks to women so they can make "informed decisions" about mammograms and breast cancer screening.
"Despite increasing dissemination of information about cancer overdiagnosis and overtreatment via both news media coverage and health-related websites, patient awareness remains low," wrote first author Rebekah Nagler, PhD, senior author Sarah Gollust, PhD, and colleagues.
But the survey results are based on overestimates of the rate of overdiagnosis, and they may actually demonstrate that women just don't think overdiagnosis and overtreatment are problems when compared with the benefits of finding early breast cancer, according to Dr. Daniel Kopans from Massachusetts General Hospital.
"The authors appear to be unaware that the claims of overdiagnosis by mammography screening are greatly exaggerated and have been repeatedly refuted," Kopans told AuntMinnie.com via email. "If you start with a false premise, and then find that those interviewed are not aware of or do not accept your false premise, then what is the value of your findings?"
Unbelievable?
In 2016, the researchers surveyed 429 U.S. women between the ages of 35 and 55. Of these women, 16.5% were aware of the potential risk of overdiagnosis from breast cancer screening and 18% were aware of the concept of overtreatment. Women younger than 40 were least likely to have heard about overdiagnosis, the group found (Medical Care, October 2017, Vol. 55:10, pp. 879-885).
Survey participants were presented with two statements regarding overdiagnosis and overtreatment:
- Some breast cancers found by mammograms are so slow-growing that they would not have caused any health problems for women in their lifetime.
- Some breast cancers that are treated would not have needed such treatment after all.
Women were asked to rank their responses to the following statements on a scale of 1 (strongly disagree) to 5 (strongly agree):
- This statement is believable.
- Overall, I agree with this statement.
- This statement gives me a strong reason to think carefully about whether I will get a mammogram.
Fewer than a quarter agreed with and found the statements to be believable, and even fewer evaluated them as strong arguments to consider in their own mammography decision-making, the authors wrote. Women who had recently had a mammogram and those with a regular source of medical care were "particularly unconvinced" by these statements.
Because many women view breast cancer screening favorably, it may be "challenging" for providers to communicate its potential harms to patients, the group concluded.
"Given the public's entrenched ... favorability toward screening, it is plausible that exposure to dissonant messages about overdiagnosis and overtreatment could have negative consequences, such as prompting patients' counterarguing and limiting their engagement in shared decision-making," the authors wrote. "Rigorous health communication research is necessary to inform communication interventions that could improve patient understanding of overdiagnosis and overtreatment, promote appropriate use of screening, and, in turn, ensure high-value care."
The current findings parallel those of a June 26 paper published in JAMA Internal Medicine, again from Gollust et al, which also indicated that women valued the benefits of mammography more than they were concerned about overdiagnosis and harms.
Right question?
An answer to the question of how to improve communication so that women understand mammography's harms isn't what's needed, according to Kopans. Instead, what's important is whether women understand mammography's benefits.
" 'Overdiagnosed,' or 'fake' cancers will be there however long screening is delayed," he said. "So this means that the only 'harm' from screening are recalls for additional evaluation. And the question that has never been answered by those who claim to have weighed the harms of mammography screening against its benefits is: How many fewer recalls are equal to allowing one woman to die unnecessarily?"