Studies suggest that digital breast tomosynthesis (DBT) not only improves cancer detection rates, it also decreases recall rates, especially in women with dense breast tissue. But it's also beneficial for women who don't have dense tissue, according to research published in the April 26 issue of the Journal of the American Medical Association.
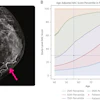
When combined with digital mammography, DBT decreased recall rates 14% and improved cancer detection rates 48% in women with dense tissue. In addition, in women with fatty breast tissue, the recall rate was 12% lower and the cancer detection rate was 30% higher.
"The message in our data is that whether a woman has dense tissue or not, tomosynthesis is beneficial," lead author Dr. Elizabeth Rafferty of L&M Radiology in West Acton, MA, told AuntMinnie.com. "We're used to incremental gains when a new technology is introduced, but these results are beyond incremental."
Parsing density
Rafferty and colleagues used data from their 2014 study, also published in JAMA, which found that adding DBT to mammography screening boosted the detection of invasive cancer by more than a third compared to mammography alone, and reduced the number of false positives by 15%.
 Dr. Elizabeth Rafferty of L&M Radiology.
Dr. Elizabeth Rafferty of L&M Radiology.For the new research, they focused specifically on DBT's efficacy across four breast density categories, assessing overall and invasive cancer detection rates and recall rates for mammography alone and for mammography with tomosynthesis. The four density categories covered tissue that was almost entirely fatty, scattered fibroglandular, heterogeneously dense, or extremely dense (JAMA, April 26, 2016, Vol. 315:16, pp. 1784-1786).
The study consisted of more than 450,000 screening mammography exams: 278,906 were digital mammography alone and 173,414 were digital mammography plus tomosynthesis. From these exams, 2,157 cancers were identified.
The researchers then created two subgroups of tissue -- dense and nondense -- from the original four categories. Women with heterogeneously dense or extremely dense tissue were put in the dense category, while those with almost entirely fatty or scattered fibroglandular tissue were placed in the nondense category.
With the combination of digital mammography plus tomosynthesis, the overall recall rate per 1,000 screens decreased from 90 to 79 in women without dense tissue, while in those with dense tissue, the overall recall rate per 1,000 screens decreased from 127 to 109, according to Rafferty and colleagues.
Recall, cancer detection, and positive predictive value (PPV) rates across the two density subgroups are shown in the following table.
| Impact of DBT on breast screening by tissue type | ||||
| Nondense tissue | Dense tissue | |||
| Digital mammo | Digital mammo + DBT | Digital mammo | Digital mammo + DBT | |
| Recalls per 1,000 screens | 90 | 79 | 127 | 109 |
| Cancers per 1,000 screens | 4.2 | 5.1 | 4.5 | 5.8 |
| Invasive cancers per 1,000 screens | 3 | 4 | 2.9 | 4.2 |
| PPV for recalls | 5.1% | 7.1% | 3.8% | 5.7% |
When Rafferty's group broke out the data for each of the four density categories, the combination of digital mammography and tomosynthesis reached statistical significance across all measures for women with scattered fibroglandular and heterogeneously dense tissue, as well as for reduced recall rates in women with extremely dense tissue.
But the results did not reach statistical significance for women with almost entirely fatty tissue across all measures, or for women with extremely dense tissue for overall and invasive cancer detection and PPV for recall.
"The combined gains [of increased cancer detection and decreased recall rates] were largest for women with heterogeneously dense breasts ... but were not significant in women with extremely dense breasts," Rafferty and colleagues wrote.
Future directions
Tomosynthesis is still a limited resource, and many practices are trying to determine whether to implement the technology and, if so, to do it across the board or targeted to specific groups of women. These study findings may help clarify these questions and suggest a way to better personalize breast cancer screening, Rafferty said.
"We have this new technology that's better than mammography alone, so how do we parse its use among women with different densities?" she said. "For women with heterogeneously dense breast tissue, tomosynthesis represents a major improvement over digital mammography, while the degree of benefit in reducing recall rate and finding invasive cancers in women with extremely dense breast tissue -- which is about 6% of all women screened -- is real, but not as large. Knowing that can help us figure out how best to serve this population."
The results of the study also raise the possibility that DBT may obviate the need for supplemental screening for the majority of women with dense tissue. More than half of U.S. states have now passed breast density notification legislation, intended to inform women with dense tissue that they should discuss with their doctor whether they need supplemental imaging for breast cancer screening -- and most of those women are referred to ultrasound. But ultrasound tends to have a high false-positive rate, which is one of the most often mentioned "harms" of mammography screening.
"Our results give us a real opportunity to explore which women might really benefit from additional imaging, and which modality is most effective," Rafferty said.
Study disclosures
The study was funded by a research grant from Hologic.